Understanding Psoriasis: A Chronic Illness

- Psoriasis
- 22 Aug 2023
Overview
What is Psoriasis?
Psoriasis is a long-term (chronic) disease, that provokes a few or several patches on the skin. It is a non-contagious immune system disease, in which the body’s fighting cells assault healthy skin cells by mistake (autoimmune). Symptoms’ onset may be sudden and last for several weeks. The treatments available to date do not cure the disease but can help treat the symptoms and improve the quality of life1Overview| Researched based study from Scirp.org
People affected by psoriasis require regular follow-up. You should seek medical attention if your condition worsens, becomes disabling, causes a change in your skin appearance, or is unimproved with treatment.
Prevalence
Psoriasis can affect everybody and at all ages, but it is most frequent towards the fifties. It concerns about 2% to 3% of the world’s population.1Overview| Researched based study from Scirp.org
Symptoms
Symptoms of Psoriasis
Psoriasis primarily affects the skin but may also affect other parts of the body, such as the joints. It commonly develops on the scalp, elbows, and knees; but can begin at an injury or trauma site—a condition called Koebner’s phenomenon.1Symptoms| Researched based study from Scirp.org The most frequent symptoms of psoriasis are:2Symptoms| Researched based study from Who.int
- Psoriatic patch: A rash with patches of varying color (very often red) and appearance, capable of bleeding, and ranging from spots of dandruff-like scaling to widespread rashes.
- Itching
- Swelling
- Burning sensation
- Skin hurts
Types
Types of Psoriasis
Five main types (forms) of psoriasis exist3Types| Researched based study from Nlm.nih.gov They include :
Psoriasis Vulgaris
- It is the most common type of psoriasis and is also called plaque psoriasis (this is what the term “psoriasis” refers to). It presents as little confined, red, itchy patches (plaques) covered with scales. There could be a few or many, and the patches can merge to cover large areas of skin. Common locations include the scalp, elbows, knees, and trunk.
Inverse Psoriasis
- Also known as flexural psoriasis, it affects the skin folds (e.g., armpits, breasts, et cetera.) and aggravates with abrasion .
Guttate Psoriasis
- This form of psoriasis mainly affects children or teenagers and some of them will develop psoriasis vulgaris once they become adults. It is often provoked by group-A streptococcal infections of the tonsils and presents as scanty, red spots with scaling on the trunk, arms, or legs.
Pustular psoriasis
- Pustular psoriasis rarely occurs. The rash presents as small skin elevations full of pus.
Erythrodermic psoriasis
- It is the least frequent type and can develop on the previous forms of psoriasis. The rash involves almost all the body surface and may cause an intense sensation of burn.
Causes
Causes of Psoriasis
The cause of psoriasis has not yet been clarified; but a few are following:
- Genes, together with some environmental conditions can elicit the disease.
- Parents can pass on the disease to their children.4Causes| Researched based study from Nlm.nih.gov
Triggers
Psoriasis Triggers
External and internal triggers can provoke the disease, Like:
- Injury to the skin, such as sunburn or an insect bite
- Infections due to streptococci or other skin infections
- Drugs (high blood pressure drugs, antimalarial drugs, etc.)4Triggers| Researched based study from Nlm.nih.gov
- Stress
- Lack of sleep
- Pregnancy: The course of psoriasis during pregnancy is uncertain, and about 23% of pregnant women experience intense flares5Triggers| Researched based study from Mayoclinic.org
Diagnosis
Diagnosis
- Your doctor will have to describe your rashes (signs and locations) in order to diagnose the disease, and might need to collect a fragment of your skin to analyze. These will help determine the type of psoriasis and exclude other diseases.
- Skin biopsy is one method of diagnosis confirmation.
- There are no special blood tests for psoriasis.2Diagnosis| Researched based study from Who.int
Complications
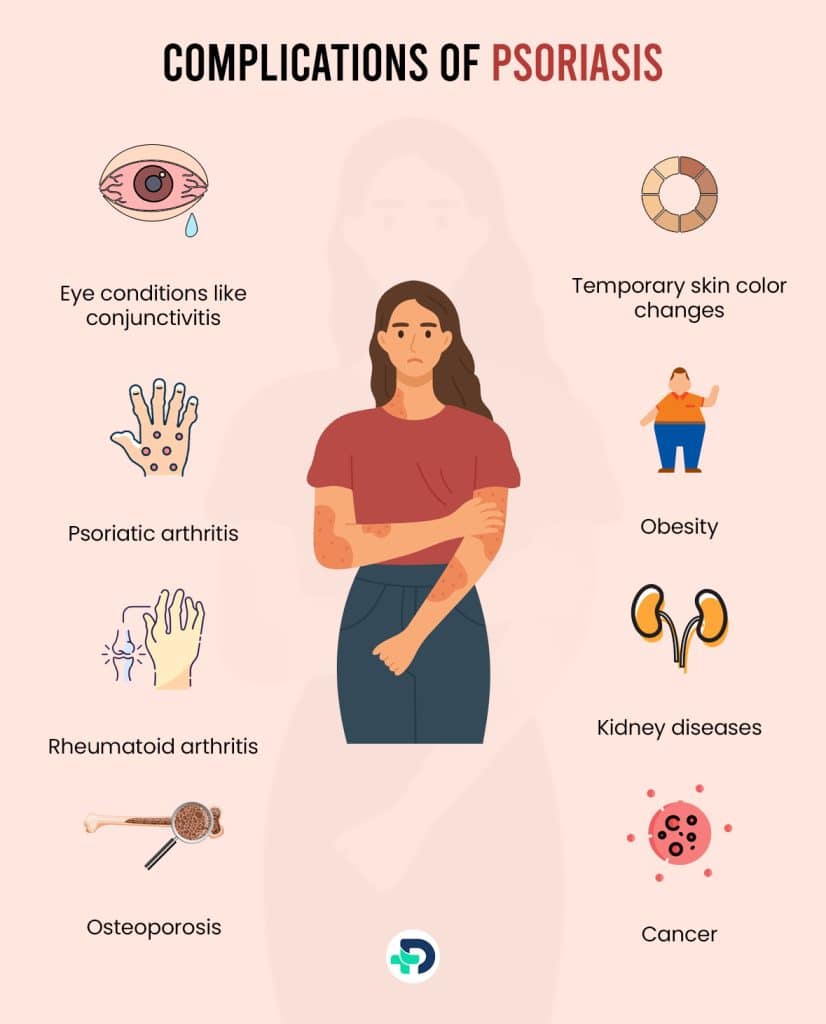
Complications of Psoriasis
The complications of psoriasis can shorten your lifetime and affect your well-being. They include:
- Psoriatic arthritis (causes pain, deformity, disability, and swelling around joints.)
- Temporary skin color changes
- Eye conditions like conjunctivitis
- Obesity, high blood pressure, type 2 diabetes, and an abnormal increase in blood lipid levels (which can increase the risk of suffering a stroke).
- Other autoimmune diseases such as rheumatoid arthritis
- Chronic obstructive pulmonary disease
- Kidney diseases
- Osteoporosis and other bone diseases
- Cancer 1Complications| Researched based study from Scirp.org ,3Complications| Researched based study from Nlm.nih.gov
Management
Management of Psoriasis
No definitive treatment exists for psoriasis.2Management| Researched based study from Who.int The goal of the treatment is to slow down the growth of skin cells and relieve the symptoms. The treatment options include creams and ointments (topical medication), light therapy (phototherapy), and oral or injectable medications
You and your doctor will choose a treatment based on your needs and the type and severity of your psoriasis. He will ensure the treatment is effective and safe for you and decide whether to use one medication or combine different medications.
First-line Treatment
Ointments and creams constitute the first-line treatment for psoriasis and are the mainstay of treatment for all forms of psoriasis. They treat mild forms of the disease.1Management| Researched based study from Scirp.org ,3Management| Researched based study from Nlm.nih.gov
- Corticosteroids: Corticosteroids are the medications of choice in the first-line treatment of psoriasis and are available as gels and lotions. Examples are hydrocortisone (Cortef®) and triamcinolone (Trianex®). Apply to the patches once a day and for a short period, because long-term use can thin the skin.
- Salicylic acid: Salicylic acid is a peeling medication (keratolytic) that removes the scales and relieves irritation and redness. It is available as shampoos or creams.
- Tar preparations: Tar preparations have a similar effect with salicylic acid—reduce scales and relieve itching and irritation—and are available as creams and oils.An example is coal tar (Betatar®).
- Vitamin D derivatives: You may use vitamin D derived medications alone or combined with corticosteroids. They include calcitriol (Vectical®), maxacalcitol (Oxarol®), and tacalcitol (Curatoderm®).
- Calcineurin blockers: Calcineurin blockers inlude tacrolimus (Astagraf®) and pimecrolimus (Elidel®). You can use them for difficult-to-treat sites, such as the skin folds or the face.
- Anthralin: Anthralin (Drithocreme®) softens the skin and reduces and prevents scales. It can be used alone or combined with corticosteroids.
Second-line Treatment
Second-line treatment treats moderate to severe forms of the disease and is for short-term use because it is harmful over long periods. It includes:1Management| Researched based study from Scirp.org ,3Management| Researched based study from Nlm.nih.gov
- Light therapy: It is an effective but time-consuming treatment that uses natural (sunlight) or artificial light. Your doctor will deliver a precise amount of light to the patches that will kill the fast-growing skin cells and relieve the symptoms. Examples include narrow-band ultraviolet B (UVB) and psoralen plus ultraviolet A (PUVA). PUVA cannot be used over long periods because it may cause skin cancer.
- Methotrexate: You may experience nausea and fatigue while taking methotrexate. Your doctor will assess your liver function and complete blood count, to ensure a long-term treatment is feasible.
- Cyclosporine: Cyclosporine has the same efficacy as methotrexate but cannot be used for more than a year because of its adverse effects—high blood pressure and kidney damage.
- Retinoids: Patients with psoriasis respond well to retinoids.An example is acitretin—a medication derived from vitamin A. Some side effects include irritation of the conjunctiva and liver.
- Fumaric acid esters: They are effective when used alone or combined with other medications, especially calcipotriol (Dovonex®); and improve the symptoms of psoriasis. An example is Fumaderm®. Common side effects include abdominal pain, nausea, diarrhea, and skin flush. Patients receiving fumaric acid esters need regular complete blood counts, liver, and kidney function tests.
Third-line Treatment
Third-line treatment1Management| Researched based study from Scirp.org ,3Management| Researched based study from Nlm.nih.gov treats moderate to severe forms of psoriasis.
- The main medications here are biologics which include adalimumab (Humira®), etanercept (Enbrel®), infliximab (Remicade®), and ustekinumab (Stelara®). They are safer in the long term compared to other treatment options.
Note that the disease remains even after the patches have gone away. The skin symptoms of psoriasis reappear in most cases when you stop the treatment—an effect known as rebound.
Lifestyle changes
Some lifestyle changes can help manage psoriasis:
- Eat healthily
- Exercise regularly
- Seek to lose weight
- Stop smoking
- Abstain from alcohol 6Management| Researched based study from Cochrane.org
Outlook
The Outlook
Psoriasis causes a huge psychological and social burden. Treatment options are available to manage the symptoms of the disease and prevent relapse, but there is no cure to date. Lifestyle changes, together with the various treatment options, can help patients with psoriasis have a better life.
Any feedback on this article?
 This Articles content was accurate
This Articles content was accurate Very Informative Article
Very Informative Article I have a question or a comment
I have a question or a comment
 This article contains inaccurate content
This article contains inaccurate content This article was not helpful
This article was not helpful I have a question or a comment
I have a question or a comment
We appreciate your helpful feedback!
Checkout our social pages
References
-
Scientific Research Publishing
Psoriasis: A Comprehensive Review on the Aetiopathogenesis and Recent Advances in Long-Term Management of Patients with Plaque Psoriasis | Overview | Complications | Management
-
World Health Organization
Psoriasis | Symptoms | Diagnosis | Management
-
National Library of Medicine
Psoriasis Pathogenesis and Treatment | Types | Management
-
National Library of Medicine
Genetic Background of Psoriasis | Causes | Triggers
-
Mayo Clinic
Psoriasis | Triggers
-
Cochrane
Lifestyle changes for treating psoriasis | Management