Malaria : A General Overview

- Malaria
- 16 Aug 2023
Overview
What is Malaria?
Malaria is a mosquito-borne illness that can be fatal to people. It is primarily distributed in tropical regions. It can be avoided and treated. This parasitic illness cannot be passed from person to person.
Malaria is a very dangerous illness spread by mosquitoes that feed on humans after becoming infected with a parasite. People who contract malaria often experience severe symptoms, including high fevers, chills, and flu-like symptoms. Malaria can prove to be a deadly disease; however, it is mostly avoidable and treatable.
Key facts
What are the key facts about Malaria?
- About 50% of the global population was susceptible to malaria in 2021.1Key facts| Researched based study from Who.int
- It was anticipated that 247 million people would become infected with malaria that year.
- In 2021, an estimated 619,000 individuals would lose their lives to malaria.
- Pregnant women and their unborn children are a prime target for malaria because of their weakened immune systems.
- Over ten thousand pregnant women and two hundred thousand newborns younger than one-year-old succumb every year due to malaria.6Facts| Researched based study from Unicef.org
Causes
Causes of Malaria
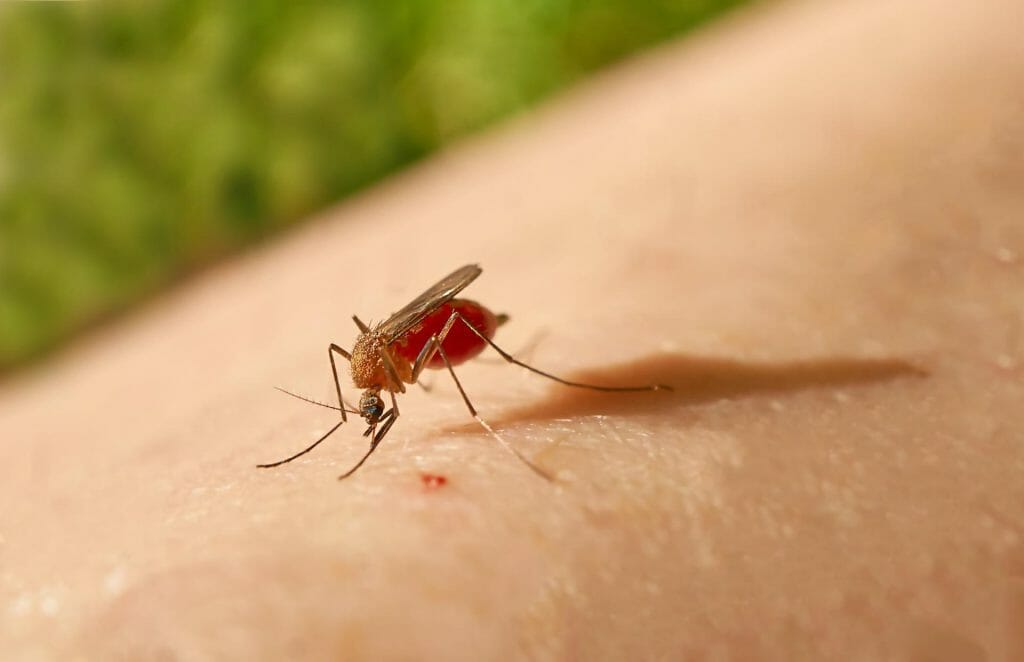
Bite of infected anopheles
A parasite called plasmodium is responsible for malaria.
- Infected anopheles mosquitoes can transmit the disease to people via a bite.
- After parasite infection, the sporozoites circulate through the body and eventually settle in the liver.
- There, they develop into parasites called merozoites and are released into the environment.
- The parasites invade the blood cells after getting into the circulatory system.5Causes| Researched based study from Nlm.nih.gov
- Common malaria symptoms are brought on by injection of merozoites into the circulatory system
- Anemia caused by RBC (red blood cell) breakdown
- The release of free hemoglobin into the bloodstream after red blood cells rupture can be harmful to other organs including the kidneys.
From a mother to her unborn baby
- Congenital malaria transmission occurs when a pregnant woman unknowingly passes the disease to her unborn child.5Causes| Researched based study from Nlm.nih.gov
Other causes
- Transfusion of infected blood
- From infected syringes
Mosquitoes can spread malaria in temperate regions, but the parasite dies off during the colder months.
Stages
Stages of Malaria
There are three distinct phases to a malaria paroxysm.5Stages| Researched based study from Nlm.nih.gov
The initial phase
- This phase lasting anywhere from 15 to 60 minutes, is marked by coldness and shivering.
Hot stage
- Following the initial phase , this stage can last anywhere from two to six hours and feature symptoms such as a high temperature (up to 41 degrees Celsius), sweating, redness, dry skin, and frequently a headache, nausea, and vomiting.
Last stage
- The last stage lasts for two to four hours and is characterized by a quick decrease in fever and profuse sweating.
The periodic febrile response seen in all forms of malaria is due to the rupture of mature schizonts. The periodicity of fever in P. vivax and P. ovale malaria is tertian (“tertian malaria”) because a brood of schizonts matures every 48 hr, whereas in P. malariae illness it is quartan (“quartan malaria”). The fever associated with falciparum malaria may occur every 48 hours, but this is not typical.5Stages| Researched based study from Nlm.nih.gov
Transmission
How is Malaria transmitted?
- The female Anopheles mosquito is the cause of the majority of cases of malarial transmission.
- Malaria can only be spread by Anopheles mosquitoes, which can only get infected after sucking the blood of a person who already has the disease.
- Malaria parasites, which are extremely minute, are transmitted from one person to another via mosquito bites.
- These parasites then combine with the mosquito’s saliva fluids and enter into the person bitten around a week later.2Transmission| Researched based study from Cdc.gov
Since the malaria parasite lives in the red blood cells of an infected person, the disease can also be spread by organ donation, blood transfusion, or the sharing of needles or syringes that have been contaminated with blood.
Transmission of malaria from mother to child can also occur during pregnancy during labor and delivery.
Symptoms
What are some Malaria symptoms?
Common symptoms of malaria are
After coming in contact with an infected mosquito, symptoms usually appear between 7 and 14 days later. For individuals, especially those who have already battled malaria, the disease may cause very minor symptoms.
- Fever, headache, and chills are the typical first indicators of malaria.
- Due to the vague nature of some malaria symptoms, early diagnosis is crucial.
- Sweats, malaise, muscle aches, nausea, and vomiting are common early symptoms.
- Malaria can swiftly worsen into a lethal condition.1Symptoms| Researched based study from Who.int
Malaria can be deadly in its most severe forms. Children under the age of 5, pregnant women, foreign travelers, and those with HIV/AIDS are at particularly high risk1Symptoms| Researched based study from Who.int
Among the severe symptoms are
- Fatigue and extreme weariness
- Reduced mental capacity
- Many fits of convulsions
- A fever, chills, and/or persistent cough jaundice (characterized by a yellowing of the eyes and skin)
- Anomalous bleeds.1Symptoms| Researched based study from Who.int
Severe symptoms necessitate prompt emergency care. In mild cases of malaria, prompt treatment can prevent complications. Malaria’s long-term effects can be devastating if the disease isn’t treated quickly, potentially leading to kidney failure, seizures, mental confusion, coma, and even death.
Complications
Long-term effects and complications of Malaria
In the absence of prompt medical attention, malaria can be lethal. Complications due to malaria can cause life-long harm and appear quickly after the disease has been detected. For this reason, prompt medical attention is required.3Complications| Researched based study from Nhsinform.scot
Anemia
- Severe anemia can result from the collapse of red blood cells due to the malarial parasite.
- In anemia, the red blood cells do not carry enough oxygen to provide to the body’s tissues.
- This can cause fatigue, dizziness, and even fainting.3Complications| Researched based study from Nhsinform.scot
Cerebral Malaria
- Malaria can occasionally cause neurological problems.
- Cerebral malaria causes brain swelling and, in severe cases, can cause irreversible brain damage.3Complications| Researched based study from Nhsinform.scot
- It may potentially result in convulsions or a coma.
Additional Complications
Malaria’s severe forms can cause other problems, such as:
- Liver failure, manifested by a yellowing of the skin and the whites of the eyes, and jaundice; shock, characterized by a precipitous drop in blood pressure
- Fluid accumulation in the lungs, medically known as pulmonary edema
- Syndrome of acute respiratory distress (ARDS)
- Symptoms of hypoglycemia (very low blood sugar)
- Kidney disease
- Spleen enlargement and rupture due to dehydration
Preterm birth
- Preterm birth and/or low birth weight are additional complications associated with malaria infection during pregnancy.
Risk factors
Risk factors of Malaria
- The risk of dying from malaria is highest in people who are repeatedly bitten by mosquitoes carrying P. falciparum.2Risk factors| Researched based study from Cdc.gov
- Very young infants, expectant mothers, and anyone traveling from malaria-free regions are more susceptible to severe malaria illness or death.
- Those who are economically underprivileged and who do not have access to medical treatment in remote locations are more in danger.
- The majority of malaria deaths, almost 90%, affect children under the age of five years and are concentrated in the sub-Saharan regions of Africa.
- If you’re feeling sick and there are reasons to suspect malaria (such as recent travel to an area where the disease is common), you should be tested right away.
Diagnosis
How is Malaria diagnosed?
The World Health Organization (WHO) suggests verifying all possible cases of malaria with microscopy or a fast diagnostic test that relies on parasites. Here are some best ways to know that a person has malaria. Doctors use the following methods to diagnose a patient:4Diagnosis| Researched based study from Medlineplus.gov
Blood Tests
- A diagnostic examination in which a small amount of your blood is inspected under a microscope for the existence of malarial parasites is the most accurate technique for you and your doctor to determine if you do or do not have malaria.
Physical exam
- An enlarged liver or spleen may be detected during a routine physical examination.
The following checks are also carried out:
- Rapid diagnostic tests are on the rise because doctors and lab workers can benefit from their convenience and efficiency.
- Smears of blood are obtained every 6-12 hours to detect malaria.
- When anemia is present, it can be shown on a CBC.
Treatment
Treatment of Malaria
The disease, its associated mortality, and its transmission can all be mitigated by prompt diagnosis and treatment.1Treatment| Researched based study from Who.int Because of the severity of the disease, malaria is always treated medically.
Malaria is treated and prevented with a wide range of pharmaceutical options. The following factors will be considered by doctors when deciding:
- Malaria subtype
- Whether or not the malaria parasite is resistant to treatment
- The patient’s age
- Weight
- Pregnancy status.
Malaria treatment often consists of the following
- Medicines like artemether-lumefantrine, which use artemisinin as part of combination therapy, tend to be the most effective.
- Only in regions where P. vivax is still sensitive to chloroquine should the parasite be treated with this drug.
- Primaquine should be used in conjunction with the primary treatment to reduce the likelihood of a recurrence of P. vivax or P. ovale infection.
- Pills are the common delivery method for medicines. For injectable medications, some patients may need to visit a clinic or hospital.
Prevention
Prevention of Malaria
If you plan on visiting a region where malaria is predominant, consult your medical examiner about preemptive medication. Follow these 5 ways to prevent malaria to stay safe: 1Prevention| Researched based study from Who.int ,4Prevention| Researched based study from Medlineplus.gov
- Avoiding mosquito bites can help reduce your risk of contracting malaria.
- In malaria-risk areas, sleep under a mosquito net.
- When it becomes dark, it’s time to break out the DEET, IR3535, and Icaridin mosquito repellents.
- Make use of vaporizers and coils.
- Install insect screens.
- Manageable vectors
- Due to its efficacy in halting new infections and slowing the spread of malaria, vector control is an essential part of control and elimination plans. Indoor residual spraying (IRS) and insecticide-treated nets (ITNs) are the two main approaches.
Other approaches may include:
Chemoprophylaxis
- Anyone planning a trip to a malaria hotspot should see a doctor well in advance of their trip.
- The doctor will decide what chemoprophylaxis medications are safe and effective to take in the desired location.
- Chemoprophylaxis medications may need to be started as early as two to three weeks before travel.
- Prophylactic medications must be taken regularly for the full duration of time spent in a malaria-risk area and for an additional 4 weeks after leaving the area, as parasites can emerge from the liver for up to a month after an infection has been avoided.
Use of Chemoprevention
- Malaria can be avoided and its effects mitigated with preventative chemotherapy, which involves the use of drugs singly or in combination to achieve this goal.
- Periodic preventive treatment during pregnancy (IPTp) and in school-aged children (IPTsc), post-discharge malaria chemoprevention (PDMC), and mass drug administration (MDA) are all examples of preventive chemotherapy.
Vaccine against Malaria
- The World Health Organization (WHO) has strongly encouraged the widespread administration of the RTS,S/ AS01 malaria vaccine to children residing in areas with intermediate to high P. falciparum malaria transmission from October 2021.1Prevention| Researched based study from Who.int
Takeaway
Key Takeaways
The parasite that causes malaria often infects the female Anopheles mosquito, which then feeds on human blood. Malaria victims frequently experience extreme illness, including high fevers, chills, and flu-like symptoms. Malaria can be fatal, but it’s typically avoidable with proper precautions.
Protozoa belonging to the genus Plasmodium are responsible for malaria. P falciparum, P vivax, P. ovale, and P. malariae are the four human-pathogenic species of Plasmodium. Plasmodium species also infect avian and mammalian hosts. Female Anopheles mosquitoes are responsible for transmitting the malaria parasite to humans through their bites.
Any feedback on this article?
 This Articles content was accurate
This Articles content was accurate Very Informative Article
Very Informative Article I have a question or a comment
I have a question or a comment
 This article contains inaccurate content
This article contains inaccurate content This article was not helpful
This article was not helpful I have a question or a comment
I have a question or a comment
We appreciate your helpful feedback!
Checkout our social pages
References
-
World Health Organization
Malaria | Overview | Facts | Symptoms | Prevention | Treatment
-
Centers for Disease Control and Prevention
About Malaria | Transmission | Risk factors
-
NHSInform
Malaria | Consequences
-
Medline Plus
Malaria | Prevention
-
National Library of Medicine
Malaria | Stages | Causes
-
UNICEF
Ten things you didn't know about malaria | Facts