Septoplasty Unveiled: Enhancing Breathing and Quality of Life

- Septoplasty
- 05 Sep 2023
Introduction
What is Septoplasty?
One of the most often done operations in otorhinolaryngology (ENT) and cosmetic surgery is nasal septoplasty. The main cause of this functional (as opposed to just aesthetic) surgery is typically a substantial and bothersome nasal airway obstruction caused by septal deviation. Endonasal, endoscopic, and open procedures are only a few of the surgical methods and techniques that have been studied.

Nasal Septum
What is a Nasal Septum?
- Nasal septum is the primary supporting structure of the external nose that divides the nasal cavity into two different nasal airways , allowing laminar airflow and warming and humidifying the air that is inspired. 1Nasal septum | Researched based study from National Institutes of Health
- Airway obstruction can result from a septal deviation because it reduces the cross-sectional area of the nasal valve.
- This may cause nasal obstruction symptoms and, in rare cases, aggravate obstructive sleep apnea symptoms.
- Epistaxis, headaches (including “Sluder syndrome” or rhinogenic headache), and face pain can all be brought on by bony spurs that develop as a result of septal displacement.
Nasal Obstruction
What happens when there is nasal obstruction?
- When your nasal passages are obstructed or you have trouble breathing through your nose, nasal obstruction results.
- Nasal obstruction can cause major issues with eating, speaking, and sleeping in addition to being uncomfortable.
- In addition to lowering productivity and raising your risk of accidents, it can lead to weariness and despair.
- The plus side is that there are several therapies that can get rid of nasal congestion and restore your ability to breathe easily.
- Among these the most common cause of nasal obstruction is deviated septum, enlarged turbinate, nasal polyps and at last the nasal tumors
Indications
Indications for a Septoplasty
- Deviated nasal septum causing airway obstruction on one or the other side of the nasal cavity 1Indications | Researched based study from National Institutes of Health
- As a part of cosmetic reasons along with septorhinoplasty
- Recurrent nasal bleed from the nasal spur
- Recurrent sleep apnea due to septal deviation
- Migraine like headache due to sinusitis which is due to septal deviation
- Septal deviation causing sleep apnea
- In pituitary fossa surgeries like trans septal transsphenoidal approach
Contraindications
Who should not undergo Septoplasty?
Acute nasal (bacterial/viral) sinus infection: 1Contraindications | Researched based study from National Institutes of Health
- Elective surgeries are usually avoided when there is an infectious etiology present, first the infection rate is brought down by using appropriate antibiotics and only when the infection is cleared, the patient is posted for septoplasty.
- Operating in bacterial contaminated zone makes patient more prone for cerebral or brain infections
Uncontrolled sugars:
- Elevated Blood sugars are good source for bacteria to thrive and multiply.
- In simple terms, bacteria usually like the increased sugar level conditions to grow, therefore controlling blood sugar levels is very important to ruin the bacterial party.
Elevated Blood Pressure:
- Increased blood pressure causes torrential hemorrhage during operation, and can lead to blood loss landing up patient into hypovolemic shock, from surgeons’ point of view it hampers surgical field, increasing the duration of the surgery.
Bleeding disorders:
- Bleeding disorders like Hemophilia A, Hemophilia B should be ruled out, because these are congenital abnormalities with clotting factor deficiencies which delays the clotting time and increased blood loss.
- Preoperative work up should be done to rule out these conditions.
- Preoperative PT/INR, Bleeding time, Clotting time and some other investigation will be useful.
Preparation
Preparation for Septoplasty
Your ENT specialist will normally perform a physical examination 2Preparation | Researched based study from Health Direct of your nostrils to verify the position of the septum, examine the sizes of each nostril, and assess how it affects your breathing in order to diagnose a deviated septum.
- Your ENT doctor will also take into account whether the deviated septum was present at birth, the result of an injury, and whether it affects your ability to sleep or your sinuses.
- They will provide you advice on how to recuperate properly from septoplasty (surgical to correct a deviated septum).
- Medication is frequently used during recovery to ease discomfort, speed up healing, and prevent infection.
- Additionally, you’ll be urged to refrain from blowing your nose and making physical contact with your nose.
Investigations done before a septoplasty
- Routine Blood Investigations
- Complete Hemogram
- Liver function tests
- Renal function tests
- HIV, HbsAg, Blood Grouping
- RBS (Random Blood Sugar), FBS and PPBS (Fasting and Post Prandial Blood Sugars), Hba1c.
- Urine Routine
- Specific Investigations according to your physician may vary from X Ray, CT scan to MRI.
Who performs Septoplasty?
- Septoplasty procedures are often performed by ENT surgeons.
- Specialists in rhinology or cosmetic surgery of the face may do revision procedures or more complicated operations, with or without rhinoplasty.
- Septoplasties are also carried out by some plastic surgeons.
- An anesthetist, a nursing scrubber, a surgical technologist, operation theater and recovery room nurses, and assistants are additional staff needed to accomplish the procedure.
Anesthesia used:
General anesthesia
- Provides you good sleep and amnesia during the procedure to make it painless with a sound sleep.
Local anesthesia
- This is usually done by expert surgeons, can be painful when compared to general anesthesia.
Procedure
Septoplasty Procedure
- Surgeons with the help of Anesthetist administer lignocaine with adrenaline to the septum, this causes local anesthesia effect and vasoconstriction which decreases blood loss and keeps the surgical field clear. 2Procedure| Researched based study from Health Direct
- When a septum is deviated, small curvilinear incision 2-3 mm is made on septal cartilage on the concave side.
- Surgeons raise the mucoperiosteal/mucoperichondrial flap exclusively on one side.
- They lift the mucoperiosteal flap on the other side of the septum and separate the septal cartilage from underlying bone
- Additional adjustments might be necessary, such as realigning the nasal spine.
- Transseptal sutures are used to fix mucoperichondrial flap.
- The nasal pack is kept at the end of the procedure, which is removed post operatively.
Post Surgical Care
Post Surgical Care
- Septal surgery is a day procedure, and the patient can return home once the sedative effects have completely worn off and if there has been no nausea following the procedure or bleeding.
- Obstructive sleep apnea patients will be better monitored overnight.
- Following a saline spray or steam inhalation, remove the nasal pack.
- If necessary, nasal splints are removed on 4th to 8th day and the nose is gently suctioned.
- The patient is observed in between one and two weeks for a postoperative evaluation and, if necessary, the removal of any splints.
- Usually, antibiotics are not necessary. Antibiotics for the prevention of staphylococcal toxic shock could be necessary if gauze packing is used to stabilize broken bone fragments.
- After surgery, there will be swelling inside your nose. For two to five days following surgery, your nose may leak and bleed a little.
- Your top lip, cheekbones, and nose can feel numb. It can take several months for the numbing sensation on the tip of the nose to go away completely.
Post Surgical self-care instructions :
- Avoid touching or rubbing your nose. Avoid blowing your nose; a few weeks of stuffiness is usual. You can snort to draw secretions back into the throat.
- If the nose becomes stuffy, drops that are prescribed by your surgeon are employed.
- To reduce pain and swelling, you can place cold packs near your eyes and nose.
- However, keep your nose dry. With a tiny towel or clean, dry cloth, wrap the ice pack. It will also assist to minimize edema to sleep on two pillows.
- Take painkillers or a prescription medication, as directed by your doctor.
- For at least 24 hours following surgery, you shouldn’t drive, operate machinery, consume alcohol, or make any significant decisions.
- You can feel drowsy from the anesthesia and find it difficult to think straight. It should take around 24 hours for the effects to fade.
- Avoid engaging in any activity that could cause you to fall or increase the pressure on the area around your face. Some of these include stooping, holding your breath, and tensing up your muscles when having a bowel movement.
- For a week or two, refrain from strenuous physical activity and heavy lifting.
- Take no showers or baths for 24 hours.
- You’ll be shown by your nurse how to clean the area around your nose using Q-tips and hydrogen peroxide.
If any of the following applies to you, Call your doctor immediately :
- Difficulty breathing
- A severe nosebleed that you are unable to stop
- Increasing or unrelieved pain, or pain for which your pain medications are ineffective
- Rigors and a high temperature
- Headaches
- Disorientation
- Neck discomfort
Complications
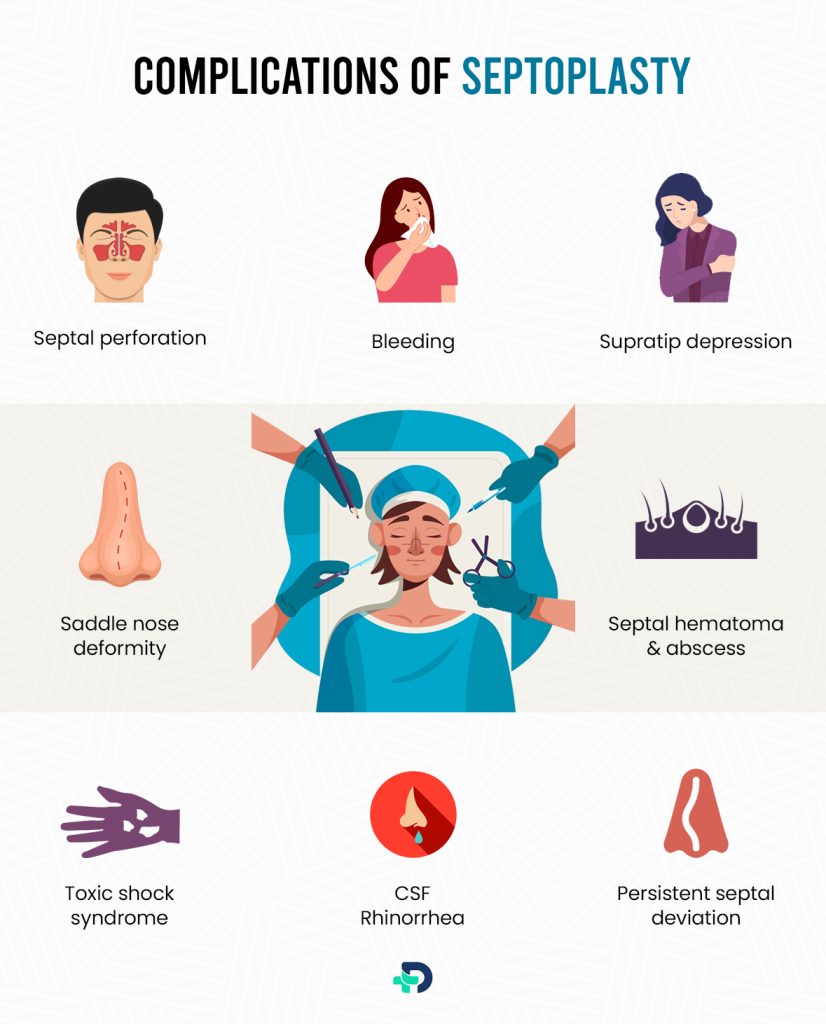
Septoplasty Complications
- Septoplasty has a very high success rate. 2Complications| Researched based study from Health Direct The surgery offers a lifelong repair of a deviated septum for the majority of patients.
- Within the initial couple of weeks following surgery, you should plan to see your healthcare practitioner for a follow-up appointment.
- This enables the interior layer of your nose to be examined to evaluate the healing process.
You will be assessed for your vulnerability to the following postoperative problems after your septoplasty:
- Bleeding
- Septal perforation
- Supratip depression
- Saddle nose deformity
- Septal hematoma and abscess
- Toxic shock syndrome
- CSF Rhinorrhea
- Persistent septal deviation
Frequently Asked Questions (FAQs) about Septoplasty
Which drugs shouldn’t be consumed before surgery?
- No ibuprofen, aspirin, or other blood thinners. Tell your physician, if you are taking any medications that thin the blood.
How much time does the process require?
- Roughly one to two hours. To account for the time, it takes to fall asleep and awaken following the treatment, add 30 minutes.
- We strive to be one-time, but surgery is unpredictable, and delays are always a possibility. Consider taking the whole day off.
Will a septoplasty treat my sleep apnea or snoring?
- No, generally. The primary goal of a septoplasty procedure is to enhance nasal ventilation. Theoretically, you ought to be able to withstand and succeed with CPAP or dental appliances better.
Takeaway
Takeaway
Surgical procedure to fix deviated nasal septum is called a septoplasty 3Takeaway | Researched based study from American Society of Plastic Surgeons . This septum is curved to one side. When this happens, your nose cannot breathe normally. The obstruction is removed when the issue is corrected, and your nasal space is returned to its usual shape. This procedure is performed as an outpatient. Although septoplasty is thought to be quite common, it still entails some hazards. Additionally, there is a chance that symptoms won’t get better. To treat your symptoms, the operation might need to be repeated. Septoplasty is a surgical procedure that returns breathing to normal. A rhinoplasty, or cosmetic surgery, may be used in specific circumstances to alter the appearance of your nose.
Any feedback on this article?
 This Articles content was accurate
This Articles content was accurate Very Informative Article
Very Informative Article I have a question or a comment
I have a question or a comment
 This article contains inaccurate content
This article contains inaccurate content This article was not helpful
This article was not helpful I have a question or a comment
I have a question or a comment
We appreciate your helpful feedback!
Checkout our social pages
References
-
National Institutes of Health
American Society of Plastic Surgeons
-
Health Direct
Preparation | Procedure | Complications
-
American Society of Plastic Surgeons
Summary