Coronary Artery Disease : Causes, Symptoms, and Management

- Coronary Artery Disease
- 14 Aug 2023
Overview
What is Coronary artery disease ?
Coronary artery disease is a disorder that involves accumulation of plaque in the arteries, which either narrows or blocks these arteries. This in turn affects the supply of blood to the heart.
Damage to the coronary arteries, the main blood vessels supplying the heart, is the leading cause of coronary artery disease (CAD). Atherosclerosis, the buildup of plaque inside the artery walls, is the main cause of coronary artery injury because it causes the arteries to narrow and become more fragile 4Overview | Researched based study from Cdc.gov

Classification
The Varieties of Coronary Artery Disease
Coronary artery disease can manifest in two distinct ways:
Stable Ischemic heart disease
- In this disease type, your coronary vessels shrink over time. Your heart will receive less oxygen-rich circulation as you age. You’re able to manage the disease on a day-to-day basis despite experiencing some signs. 1Classification | Researched based study from Clevelandclinic.org
Acute coronary syndrome
- When a plaque in the coronary artery bursts, it can cause a blockage to develop and cut off the blood supply to the heart. This sudden obstruction leads to cardiac arrest.1Classification | Researched based study from Clevelandclinic.org
Symptoms
Symptoms of coronary artery disease
Coronary artery disease may not show any signs at all for quite some time. Plaque can develop slowly over many years or even decades. However, you may experience slight discomfort as your vessels begin to constrict. Your heart is working harder to supply your body with oxygen-rich blood, as evidenced by these signs.
Some of the signs of chronic CAD are:
Stable angina
- The most prevalent form of chest pain is stable angina. Temporary cardiac pain or soreness that occurs and disappears at regular intervals is called stable angina. It is most obvious when you are exerting yourself physically or experiencing strong emotions. When you sleep or take nitroglycerin, the pain disappears.
Dyspnea
- Some individuals experience dyspnea, or shortness of breath, even when engaging in relatively mild physical exercise.
A heart attack
It can be the first sign of coronary artery disease. Heart attack symptoms include 4Symptoms | Researched based study from Cdc.gov
- Physical distress in the chest (angina). There is a wide spectrum of symptoms associated with angina. Heavy, tight, pressing, pressing, pressure, hurting, numbness, burning, swelling, squeezing, or mild pain are all possible descriptions. You may start to feel pain in your shoulder, arm, neck, back, or jawline.
- Problems inhaling or a feeling of being short of breath.
- Experiencing vertigo or dizziness.
- Palpitating heart
- Tiredness.
- Nausea, or puking.
- Weakness.
More often than not, women and AFAB individuals will also exhibit additional, unusual signs such as 1Symptoms| Researched based study from Clevelandclinic.org
- Before the heart attack, the patient experiences shortness of breath, lethargy, and sleeplessness.
- Severe discomfort all over their body.
- Pulse quickening.
- Feeling hot or flushed
Heart failure develops when the heart is unable to circulate enough blood around the body due to a decrease in blood flow caused by coronary artery disease.
Causes
Causes of coronary artery disease
- Coronary artery disease is brought about by atherosclerosis. Plaque builds up over time in vessels, causing atherosclerosis and making the vessels constricted and inflexible. Cholesterol, toxins, calcium, and fibrin make up plaque. 2Causes | Researched based study from Mayoclinic.org
- Plaque has the potential to clog or harm your vessels, reducing or preventing blood movement to a given area of your body. Plaque in the coronary vessels reduces blood flow to the cardiac muscle. That means your heart is starved for air and nutrition and can’t function optimally. Myocardial occlusion describes this problem which causes pain in the thorax (angina) and increases the likelihood of a heart attack.
- Plaque accumulation in the coronary arteries is associated with atherosclerosis, which can also occur in other vessels. Carotid artery disease and peripheral artery disease are two potential outcomes.
Risk
Risk factors associated with coronary artery disease
The following are other potential contributors to coronary artery disease besides elevated cholesterol. 2Risk | Researched based study from Mayoclinic.org
- Insulitis, or intolerance to insulin
- Hypertension
- Lack of physical activity (sedentary lifestyle)
- Tobacco and cigarette use
Diagnosis
Diagnosis of coronary artery disease
Diagnostic procedures and patient history help doctors determine if coronary artery disease is present.
Examiners will do the following during a comprehensive medical examination
- Take a blood pressure reading.
- Use a stethoscope to take note of your pulse.
- Inquire as to the nature and duration of your symptoms. 1Diagnosis | Researched based study from Clevelandclinic.org
- Find out about your health background.
- Inquire about your way of living.
- Inquire about your ancestry and background. They will want to know if anyone in your immediate family has cardiac disease.
- Your healthcare practitioner can use this data to calculate your risk for cardiovascular disease. 1Diagnosis | Researched based study from Clevelandclinic.org
Procedures for identifying coronary artery disease
To identify CAD, your doctor may also suggest a series of procedures to evaluate heart health. Some examples are: 3Diagnosis| Researched based study from Nlm.nih.gov
- The risk of developing CAD can be assessed by testing blood for specific components that might harm your arteries or increase your risk of CAD.
- Catheterization of the heart is performed to diagnose or confirm CAD by inserting catheters into the coronary arteries. This is the most reliable diagnostic for detecting coronary artery disease.
- CT coronary angiogram: using CT and contrast gas to see your beating heart in three dimensions. Locates coronary artery obstructions.
- A coronary calcium scan quantifies how much calcium is present in the coronary artery walls. This doesn’t tell you if you have major obstructions, but it does tell you if you’re at risk for coronary artery disease.
- An echocardiogram (echo) is a test that uses sound pulses to assess the health of your heart.
- In an electrocardiogram (EKG or ECG), the electrical activity of the heart is recorded. cardiac assaults, ischemia, and irregular cardiac rhythms can all be detected.
- The stress test measures the heart’s reaction to physical exertion. It is capable of identifying the presence of angina and coronary artery obstructions.
- A chest X-ray is also performed to create images of the lungs, heart and other organs located in the chest.
Management
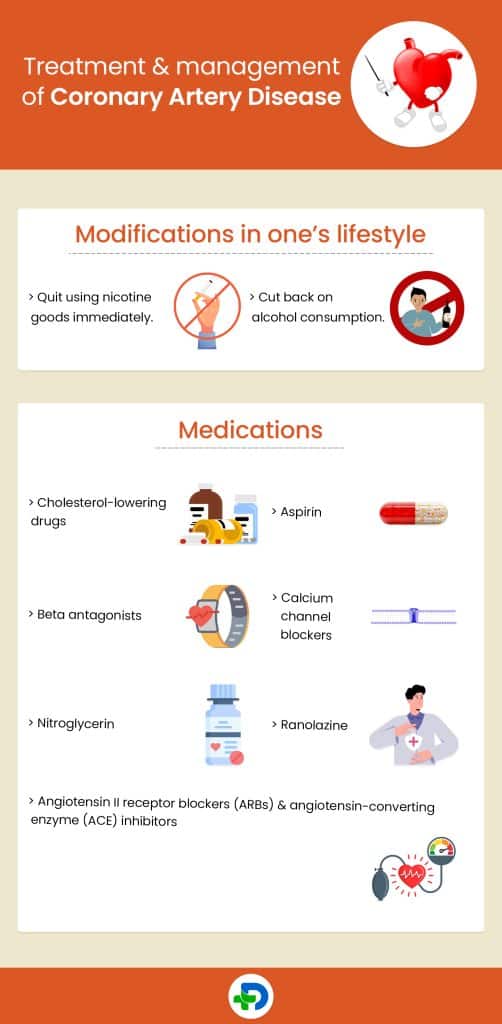
Treatment and management of coronary artery disease
Changes in living, the control of risk factors, and medication are common components of treatment for CAD. Medical treatment or operation might also be helpful for some individuals.
The optimal course of therapy for you will be discussed with you by your doctor. If you want to reduce your chance of severe problems from CAD, you must stick to your treatment strategy.
Modifications in one’s lifestyle
Modifying one’s way of life can be very helpful in controlling CAD. Among these alterations are: 1Management| Researched based study from Clevelandclinic.org
- Quit using nicotine goods immediately.
- Low-sodium, low-saturated-fat, low-trans-fat, and low-sugar diets are recommended for optimal cardiac health.
- Research shows that following a Mediterranean diet can reduce your chances of having a heart attack or stroke.
- Try to stroll for 30 minutes, five days a week, or engage in other forms of physical activity.
- Cut back on alcohol consumption.
You should consult your doctor before beginning any new form of physical activity. You can also get advice on making specific adjustments to your living from your provider. Your doctor may suggest seeing a nutritionist to talk about meal plans and ways to quit smoking.
Medications
Coronary artery disease medication can assist with risk factor management and discomfort relief. One or more of the following pharmaceuticals may be recommended by your doctor. 1Management| Researched based study from Clevelandclinic.org
Cholesterol-lowering drugs
- Plaque accumulation in the vessels and bad cholesterol can be lowered with medication. Statins, niacin, fibrates, and bile acid sequestrants are all examples of such medications.
Aspirin
- In order to avoid blood blockages, aspirin thins the blood. Some individuals may benefit from taking low-dose aspirin daily for the main prevention of cardiovascular disease.
- Stomach and intestinal hemorrhage are among the most severe adverse effects of daily aspirin use. Do not begin regular aspirin use without first consulting your doctor. 1Management| Researched based study from Clevelandclinic.org
Beta antagonists
- These medications are used to reduce the pulse rate. The blood pressure is also lowered by them. After a heart attack, beta blockers may lessen the likelihood of another one happening.
Calcium channel blockers
- If you have trouble tolerating beta blockers or if they are ineffective, your doctor may prescribe an alternative. In some cases, medications that inhibit calcium channels can alleviate chest discomfort.
Angiotensin II receptor blockers (ARBs) and angiotensin-converting enzyme (ACE) inhibitors
- The blood pressure is reduced by these medications. They might slow the progression of coronary heart disease. 1Management| Researched based study from Clevelandclinic.org
Nitroglycerin
- The vessels in the heart are enlarged by this drug. It can be used to lessen or eliminate lung discomfort. You can get nitroglycerin in the form of a tablet, an aerosol, or a patch.
Ranolazine
- Potential relief from chest discomfort with this drug is noted. In some cases, it may be given in place of a beta blocker. 1Management | Researched based study from Clevelandclinic.org
Surgical and Medical Procedures
Certain patients with coronary artery disease require medical intervention, such as:
- Coronary angioplasty is another term for percutaneous coronary intervention (PCI). Small incisions are made. Your doctor will inflate a tiny balloon and use it to prop open the obstructed artery so blood can once again circulate more freely. To keep the artery accessible, your doctor may also place a stent. 4
- Coronary artery bypass grafting (CABG) is a procedure in which a new artery is created to reroute blood flow around a blocked artery. This “detour” helps get the blood pumping again to the heart. When multiple coronary arteries are completely blocked, CABG is a lifesaver. 4Management | Researched based study from Cdc.gov
Your doctor will advise you on which of these treatments is most appropriate for you.
Prevention
How to prevent coronary artery disease?
Coronary artery disease prevention is not always possible. This is due to the reality that you can do nothing to prevent certain dangers. However, there are many things you can do to lessen the odds. Once you’ve been diagnosed with CAD, many of the measures you take to lower your risk will also aid in managing your disease.
Managing your risk factors for CAD may help you experience less severe symptoms and slower development of the disease. Manage the following conditions with the help of your examiner:
- Diabetes.
- Hypertension.
- Poor LDL levels.
- High levels of lipids (hypertriglyceridemia).
- Overweight/obesity.
The following will help reduce your chance of developing coronary artery disease and stop its progression
Resolve to end your use of nicotine products entirely
- It takes more than sheer determination to break free from the grip of addiction. That’s why finding helpful tools and communities of people to lean on is crucial. Inquire about local referrals from your service supplier. 1Prevention| Researched based study from Clevelandclinic.org
Maintain a diet low in saturated fat and cholesterol.
- This means staying away from junk food that is rich in sugar, salt, saturated fat, and fatty fat. Refined carbohydrate intake must be restricted as well. Swap these out for whole cereals (like wheat bread and brown rice). Understanding the relationship between diet and lipids is also crucial. 1Prevention | Researched based study from Clevelandclinic.org
Be sure to get enough rest
- Seven to nine hours of good slumber per night is ideal for most people. Get the restful sleep your heart needs by discussing sleep hygiene with your doctor. 1Prevention | Researched based study from Clevelandclinic.org
Uphold a reasonable weight
- Get in touch with your doctor and discuss your optimal weight. Discuss your weight loss objectives with your doctor and work together to achieve them. Make permanent adjustments to your way of living that you can actually stick to. 1Prevention | Researched based study from Clevelandclinic.org
Get your heart disease risk assessed
- You should start going to your doctor for screenings when you turn 20. You can expect your doctor to check vital signs like blood pressure and body mass index. They may also employ a heart disease risk tool to make prognoses.
Reduce your drinking
- Alcohol abuse can cause cardiac problems. No one, especially men and those who are AMAB, should imbibe more than two beverages per day. Women and individuals with AFAB should stick to a daily maximum of one alcoholic beverage. However, cutting back on your alcohol consumption is preferable. 1Prevention | Researched based study from Clevelandclinic.org
Get out and about more
- Maintaining a weekly fitness regimen of 150 minutes is recommended (for example, 30-minute walks five days a week). The healthier a lifestyle you maintain, the better for your heart health. Naturally, you should consult your provider to determine a secure exercise level for you. 1Prevention | Researched based study from Clevelandclinic.org
Take your medicine as directed
- Medication plays a crucial role in lowering the chance of CAD and avoiding heart attacks in people who have already been identified with the condition. Many of these drugs require constant use for the rest of one’s life. Learn how they work to avoid unfortunate situations and potentially add years to your life.
Outlook
Outlook
According to the Centers for Disease Control and Prevention, coronary artery disease is the most prevalent form of heart illness among American adults, affecting roughly 18.2 million people. It is difficult for the coronary arteries, the main blood channels supplying the heart, to deliver enough blood, oxygen, and nutrition to the heart muscle. Coronary artery disease is typically caused by cholesterol accumulation in the heart’s vessels and inflammation.
Avoiding CAD can be greatly aided by adopting a healthy lifestyle that includes eating well, maintaining a healthy weight, and engaging in plenty of physical exercise. The best way to treat ischemic heart disease and avoid further complications is to adopt a heart-healthy lifestyle, take medication, or undergo surgery.
Any feedback on this article?
 This Articles content was accurate
This Articles content was accurate Very Informative Article
Very Informative Article I have a question or a comment
I have a question or a comment
 This article contains inaccurate content
This article contains inaccurate content This article was not helpful
This article was not helpful I have a question or a comment
I have a question or a comment
We appreciate your helpful feedback!
Checkout our social pages
References
-
Cleveland Clinic
Coronary Artery Disease | Classification | Management | Prevention
-
Mayo Clinic
Coronary artery disease | Causes | Risk
-
National Library for Medicine
Coronary artery disease | Diagnosis
-
Centers for Disease Control and Prevention
Coronary Artery Disease (CAD) | Overview | Symptoms