Dead Arm Syndrome: Everything You Need About

- Arm Pain
- 29 Sep 2023
Description
Dead Arm Syndrome
Dead Arm Syndrome, also referred to as Brachial Neuritis or Parsonage-Turner Syndrome, is an infrequent neurological disorder characterized by a complex set of symptoms involving sudden and severe pain in the shoulder and arm, often followed by muscle weakness and atrophy. This condition primarily affects the brachial plexus, an intricate network of nerves originating from the cervical (neck) and thoracic (upper back) regions of the spinal cord, which extend and branch out to control the muscles and convey sensory information in the upper limb.
Anatomy
Anatomy of the Brachial Plexus
The brachial plexus is composed of five major nerves: the axillary nerve, musculocutaneous nerve, radial nerve, median nerve, and ulnar nerve. Each of these nerves plays a crucial role in the function of the shoulder, arm, forearm, and hand. When the brachial plexus is compromised, as is the case in Dead Arm Syndrome, it can result in a wide range of symptoms affecting both motor (muscle control) and sensory (feeling) functions.
Dead Arm Syndrome is often described as a neuropathy due to its association with nerve damage. This condition involves inflammation and damage to peripheral nerves, particularly those within the brachial plexus. The exact mechanisms underlying the development of this syndrome remain a subject of ongoing research and investigation.
Incidence
Incidence of Dead Arm Syndrome
Dead Arm Syndrome is considered an exceedingly rare condition, with an estimated incidence rate of approximately 1 in 100,000 individuals. This low incidence rate makes it an infrequently encountered disorder in clinical practice. It can, however, affect individuals of all ages, including children, but it is most frequently diagnosed in adults between the ages of 20 and 60.
The rarity of this syndrome necessitates a high degree of clinical suspicion when individuals present with symptoms suggestive of Dead Arm Syndrome. Healthcare providers should remain vigilant, as early diagnosis and appropriate management are pivotal for optimizing outcomes.
Causes
Causes of Dead Arm Syndrome 1 Causes | Researched based study from National Institutes of Health
The underlying causes of Dead Arm Syndrome continue to be a subject of intense research, and the condition is not always associated with a specific, easily identifiable trigger. While no single cause has been definitively established, several factors and potential triggers have been associated with the onset of this syndrome:
Viral Infections:
In some cases, Dead Arm Syndrome has been linked to prior viral infections, notably upper respiratory infections or the flu (influenza). It is believed that the immune system’s response to these infections can lead to inflammation within the brachial plexus and subsequent nerve damage.
Vaccinations:
Rarely, vaccinations that contain tetanus toxoid (a component used in some vaccines) have been associated with the development of Dead Arm Syndrome. This is presumed to result from an autoimmune response triggered by the vaccine.
Trauma or Injury:
Physical trauma or injury to the shoulder or upper arm, such as falls, sports-related injuries, or motor vehicle accidents, has been identified as a potential precipitating factor. Trauma can directly damage the nerves of the brachial plexus or induce an inflammatory response leading to nerve damage.
Surgical Procedures:
Certain surgical procedures, especially those involving the shoulder area, can increase the risk of developing Dead Arm Syndrome. This may occur due to nerve compression during surgery or other complications related to the procedure.
Autoimmune Reactions:
In some individuals, there may be a genetic predisposition or other factors that make them more susceptible to autoimmune reactions, wherein the immune system mistakenly attacks and damages the nerves of the brachial plexus.
Genetic Factors:
While not a direct cause, there may be genetic factors that influence an individual’s susceptibility to nerve damage or their ability to recover from it. These genetic factors can make some individuals more prone to developing Dead Arm Syndrome.
The complexity of potential triggers underscores the need for thorough evaluation by healthcare professionals to identify the underlying cause in each case. It is important to note that in many instances, the precise cause remains elusive.
Symptoms
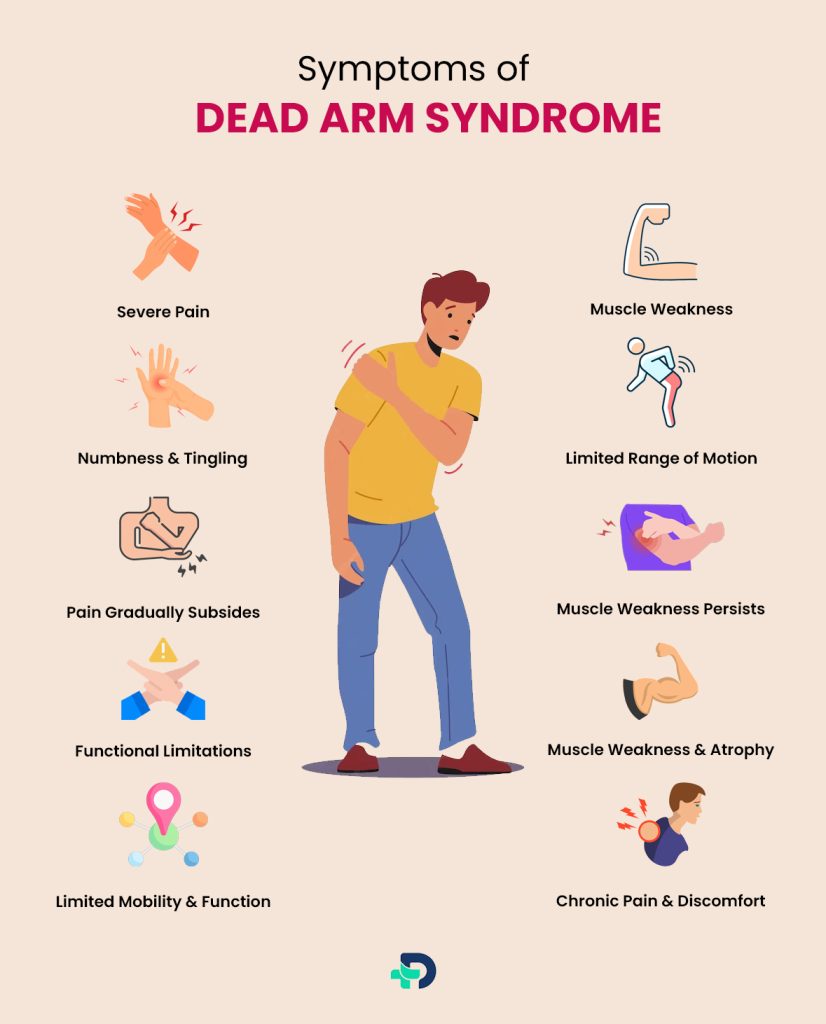
Symptoms of Dead Arm Syndrome 2 Symptoms | Researched based study from Mayo Clinic
The symptoms of Dead Arm Syndrome typically progress through three distinct phases, each characterized by specific clinical features:
1) Acute Phase:
The acute phase marks the initial onset of Dead Arm Syndrome and is typically the most dramatic phase:
Severe Pain: Individuals often experience sudden and excruciating pain in the shoulder and upper arm. This pain is frequently described as burning, stabbing, or electric shock-like in nature. It can be severe enough to awaken individuals from sleep and may be aggravated by even minor movements.
Muscle Weakness: Alongside the pain, there is muscle weakness in the affected arm, leading to difficulty in performing simple tasks. Everyday activities such as lifting objects, reaching overhead, or even holding a cup may become exceedingly challenging.
Numbness and Tingling: Many individuals report numbness or tingling sensations, medically termed paresthesia’s, in the affected arm. These sensations are often indicative of nerve involvement.
Limited Range of Motion: Due to the pain and muscle weakness, there is often a limited range of motion in the shoulder. Individuals may struggle to lift their arm, dress themselves, or perform other routine movements.
2) Subacute Phase:
The subacute phase represents a transition from the acute phase and is marked by the following features:
Pain Gradually Subsides: The intense pain experienced during the acute phase gradually subsides, although it may not completely disappear. Some individuals may experience lingering pain or discomfort.
Muscle Weakness Persists: Muscle weakness and atrophy become more noticeable during this phase, as muscle wasting continues due to disuse and nerve damage.
Functional Limitations: Individuals may find that they have difficulty performing everyday tasks, such as brushing their hair, reaching for objects, or carrying out basic self-care activities. Weakness in the affected arm may become increasingly evident.
3) Chronic Phase:
The chronic phase is the longest-lasting phase and may persist for an extended period:
Persistent Muscle Weakness and Atrophy: In the chronic phase, individuals often experience persistent muscle weakness and muscle atrophy. Muscle atrophy refers to the loss of muscle mass, which can result from disuse or nerve damage. The affected arm may visibly shrink in size and lose strength.
Limited Mobility and Function: Limited mobility and functional deficits in the affected arm may persist, impacting an individual’s ability to perform daily activities. This can lead to a reduction in quality of life.
Chronic Pain and Discomfort: Many individuals continue to experience chronic pain and discomfort, which can vary in intensity but often remains a constant presence. Managing this chronic pain becomes a central focus for healthcare providers and individuals alike.
The evolving nature of Dead Arm Syndrome underscores the importance of early diagnosis and the necessity for a comprehensive management strategy to address each phase effectively.
Complications
Complications of Dead Arm Syndrome
Dead Arm Syndrome, if left untreated or misdiagnosed, can lead to several complications that profoundly affect an individual’s physical and psychological well-being:
Permanent Muscle Weakness and Atrophy:
One of the most significant complications of Dead Arm Syndrome is the development of permanent muscle weakness and muscle atrophy in the affected arm. The ongoing damage to the brachial plexus and disuse of muscles can lead to irreversible changes in muscle structure and function. Muscle atrophy, in particular, can result in a noticeable reduction in the size and strength of the affected arm.
Chronic Pain and Discomfort:
The persistence of pain is a hallmark complication of Dead Arm Syndrome. Chronic pain can have a profound and adverse impact on an individual’s daily life. It may necessitate ongoing pain management strategies and often leads to reduced mobility and physical activity. Additionally, chronic pain is associated with psychological distress, including anxiety and depression, which further compounds the burden of the condition.
Loss of Function and Mobility:
The progressive muscle weakness and limited range of motion in the affected arm can lead to a loss of function. Individuals may struggle to perform routine activities, such as lifting objects, dressing themselves, or carrying out basic self-care tasks. Loss of function can significantly impact an individual’s independence and overall quality of life.
Psychological Distress:
Coping with chronic pain, physical limitations, and the uncertainty of the condition can contribute to emotional and psychological distress. Many individuals with Dead Arm Syndrome experience anxiety and depression, which can further exacerbate their symptoms and impact their overall well-being. Addressing these psychological aspects of the condition is an integral part of comprehensive care.
To mitigate these complications, a multidisciplinary approach to pain management, rehabilitation, and psychological support is essential. Healthcare providers work collaboratively to address both the physical and emotional aspects of the condition.
Management
Management of Dead Arm Syndrome
The management of Dead Arm Syndrome encompasses a comprehensive approach aimed at relieving symptoms, restoring function, and preventing further complications. Treatment strategies are typically tailored to the individual’s specific needs and the phase of the condition they are experiencing.
Pain Management:
i. Nonsteroidal Anti-Inflammatory Drugs (NSAIDs):
During the acute phase, healthcare providers may prescribe nonsteroidal anti-inflammatory drugs (NSAIDs) to alleviate pain and reduce inflammation in the affected area. NSAIDs can help manage pain and improve comfort, although they may have limitations in controlling severe neuropathic pain.
ii. Physical Therapy:
Physical therapy is a cornerstone of treatment for Dead Arm Syndrome. Physical therapists specialize in helping individuals regain mobility and function in the affected arm. Therapeutic exercises, stretches, and techniques are tailored to each patient’s specific needs and limitations.
iii. Local Anesthetic or Corticosteroid Injections:
In some cases, healthcare providers may recommend local anesthetic or corticosteroid injections to target specific nerve or muscle regions that are the source of pain. These injections can provide temporary relief and may be repeated as needed.
Supportive Care:
i. Rest and Immobilization:
During the acute phase, it is crucial to provide rest and immobilization to the affected arm to prevent further injury and promote healing. Immobilization may be achieved through the use of a sling or brace.
ii. Assistive Devices:
Assistive devices, such as slings, braces, or orthotic devices, may be recommended to support the arm and reduce strain, especially when performing daily activities.
iii. Occupational Therapy:
Occupational therapists play a pivotal role in helping individuals regain their ability to perform daily activities independently. They work with patients to adapt to their condition and develop strategies for accomplishing tasks.
Surgery:
In select cases, surgical intervention may be considered, especially when conservative measures do not yield the desired results or when there is evidence of nerve compression or significant muscle atrophy. Surgical options may include:
i. Nerve Decompression:
Nerve decompression procedures aim to relieve pressure on compressed nerves within the brachial plexus. This can involve releasing tight structures or removing sources of compression.
ii. Tendon Transfers:
Tendon transfers may be considered to improve muscle function and overall function in the affected arm. During this procedure, tendons from other muscles are relocated to compensate for impaired muscles.
The choice of treatment modality depends on the individual’s specific needs, the phase of the condition, and the assessment of healthcare providers. Treatment plans are often tailored to address both the pain and functional limitations associated with Dead Arm Syndrome.
Side Effects
Side Effects of Treatment for Dead Arm Syndrome
While the primary goal of treatment for Dead Arm Syndrome is to alleviate pain, improve function, and prevent complications, it is important to be aware of potential side effects associated with various treatment modalities:
a. Gastrointestinal Irritation or Bleeding:
When taking NSAIDs, individuals may experience gastrointestinal irritation, which can manifest as symptoms such as abdominal pain, indigestion, or nausea. In rare cases, prolonged use of NSAIDs may lead to gastrointestinal bleeding, which is a serious but uncommon side effect. To mitigate these risks, it is crucial to take NSAIDs as prescribed and under the supervision of a healthcare provider.
b. Temporary Weakness or Discomfort:
Following corticosteroid injections, individuals may experience temporary weakness or discomfort in the injected area. These sensations typically resolve within a few days but should be reported to the healthcare provider if they persist or worsen.
c. Surgical Risks:
In cases where surgery is recommended, there are inherent surgical risks to consider. These risks may include infection, scarring, or anesthesia-related complications. It is imperative for individuals to have a comprehensive discussion with their surgeon to understand the potential risks and benefits of the surgical procedure.
Monitoring and managing these side effects is an integral part of the overall treatment plan for Dead Arm Syndrome. Healthcare providers work closely with patients to address any adverse effects promptly.
FAQs
Dead Arm Syndrome – Frequently Asked Questions
Q. Can Dead Arm Syndrome be cured?
Dead Arm Syndrome cannot always be cured as it depends on various factors, including the extent of nerve damage and the individual’s response to treatment. However, with early diagnosis and appropriate treatment, many individuals can effectively manage symptoms, regain function, and improve their quality of life. Treatment focuses on alleviating pain, restoring function, and preventing further complications.
Q. How long does recovery take?
The recovery period for Dead Arm Syndrome can vary significantly from one individual to another. It depends on factors such as the severity of nerve damage, the effectiveness of treatment, and the individual’s overall health. Some individuals may experience improvement within several months, while others may require years of rehabilitation to regain full function.
Q. Is Dead Arm Syndrome contagious?
No, Dead Arm Syndrome is not contagious. It is a neurological condition caused by various triggers, including viral infections, trauma, or autoimmune reactions. It is not transmitted from person to person.
Q. Can it affect both arms simultaneously?
While it is rare, Dead Arm Syndrome can affect both arms simultaneously in some cases. This occurrence is even more uncommon and may present unique challenges in terms of management and rehabilitation.
Q. Can it recur after recovery?
While recurrence of Dead Arm Syndrome is possible, it is uncommon. Individuals who have experienced this syndrome should continue with follow-up care and monitoring to detect and address any potential recurrence or complications promptly.
Conclusion
Dead Arm Syndrome – Individualistic Care is Needed
In conclusion, Dead Arm Syndrome is a complex neurological disorder characterized by acute, severe pain in the shoulder and arm, followed by muscle weakness and atrophy. Early diagnosis and a comprehensive treatment plan tailored to the individual’s needs are essential for managing symptoms, restoring function, and preventing complications. This syndrome, although challenging, can often be effectively managed with the right approach and the support of healthcare professionals.
Any feedback on this article?
 This Articles content was accurate
This Articles content was accurate Very Informative Article
Very Informative Article I have a question or a comment
I have a question or a comment
 This article contains inaccurate content
This article contains inaccurate content This article was not helpful
This article was not helpful I have a question or a comment
I have a question or a comment
We appreciate your helpful feedback!
Checkout our social pages
References
-
National Institutes of Health
Causes
-
Mayo Clinic
Symptoms