Ear Infections : Understanding the Symptoms, Causes, and Management

- Ear Infections
- 27 Sep 2023
Overview
What is an ear infection ?
People of all ages, from newborns to adults, are susceptible to ear infections, which are frequent illnesses. Due to inflammation and infection in the middle ear, it is a painful condition. Both viruses and bacteria, in particular Streptococcus pneumoniae and Haemophilus influenzae, can cause ear infections. A blockage of your Eustachian tubes, which results in fluid accumulation in your middle ear, is a common cause of them.
Types
Types of Ear Infection
Ear infections come in a variety of forms and can affect various ear structures. The two most typical kinds of ear infections are as follows:
Acute Otitis Media
- This condition is brought on by a virus or bacteria that causes pus to accumulate behind the eardrum. If left untreated, this may result in discomfort, pressure, and in some cases, permanent hearing loss.
Chronic otitis media
- This ongoing infection affects the middle ear.
- The fluid that has been trapped behind the eardrum for months is what is causing the middle ear inflammation. It may contribute to the recurrence of infections such as acute otitis media.1Types | Researched based study from Nationwidechildrens.org
Otitis externa
- Often known as swimmer’s ear, is an ear infection that affects the ear canal, which connects your inner ear to your outer ear. It can be a fungal or bacterial infection.2Types | Researched based study from Vic.gov.au
Mastoiditis
- Occasional ear infections can lead to this unusual condition known as mastoiditis, which develops when the infection travels to the mastoid bone behind the ear.
Petrositis
- When an ear infection spreads to the temporal bone, the bone that surrounds the ear, it can result in this dangerous consequence.3Types | Researched based study from Medlineplus.gov
Labyrinthitis
- Labyrinthitis is an illness or inflammation of the labyrinth, which controls hearing and balance, in the inner ear. An inflamed labyrinth or one of the labyrinth’s nerves can impact hearing and balance.4Types | Researched based study from Clevelandclinic.org
Causes
Causes of Ear Infection
A bacterial or viral infection is typically what causes an ear infection. An ear infection can be brought on by a variety of factors, such as the following:
Upper respiratory illnesses
- Ear infections can result from colds, the flu, and sinusitis because these conditions cause a buildup of mucus that causes the Eustachian tube to become irritated and swollen.
Changes in air pressure
- The Eustachian tube may become blocked during air travel, which could be uncomfortable and lead to ear infections if the tube is unable to alter to the differential pressure.
Exposure to irritants
- The lining of the nasal passages and Eustachian tube can become irritated by irritants like pollutants and cigarette smoke, which raises the risk of infection.
Water exposure
- Exposure to water, such as swimming or bathing, can increase the risk of developing a swimmer’s ear.5Causes| Researched based study from Clevelandclinic.org
Pacifier use
- Ear infections are most commonly found in newborns due to their short eustachian tubes, also because the sucking motion can cause negative pressure in the middle ear, leading to fluid buildup.6Causes| Researched based study from Pennmedicine.org
Genetics
- Family history of chronic ear infections or a structural abnormality of the ear, can be considerable reasons for ear infection.
Symptoms
Symptoms of Ear Infection
Depending on the infection’s nature and location within the ear, the symptoms of an ear infection can change. Below is a list of a few of them.
Trouble sleeping
- Particularly for young children who might have problems expressing their discomfort, ear aches can make it difficult to fall asleep.
Fever
- Chills and sweating may accompany a moderate or medium fever.
Pain
- An ear infection that ranges in severity from mild to severe and gets worse at night while lying down is frequently accompanied by pain.
Difficulty hearing
- Due to fluid buildup in the middle ear, which prevents sound waves from getting to the inner ear, an ear infection can temporarily impair hearing.7Symptoms | Researched based study from Mayoclinic.org
Drainage from the ear
- Pus or fluid may occasionally discharge from the ear as a result of an ear infection. The liquid could be green or yellow in color and smell bad.
Dizziness
- Vertigo, nausea, and dizziness are all symptoms of inner ear infections that can make you feel as though you’re spinning or losing your equilibrium.
Ear fullness
- The sense of fullness or stuffiness inside the ear is known as ear pressure which occurs when tube (Eustachian) stops working.
Treatment
Treatments for Ear Infection
The type of infection and its severity determine how to treat an ear infection. Some of them consist of:
Pain relief medications
- Medicines like acetaminophen or ibuprofen can help to reduce fever and pain brought on by ear infections.8Treatment | Researched based study from Entcolumbia.org
Antibiotics
- Can be used to kill the bacteria causing the illness and are often prescribed for bacterial ear infections.
Ear drops
- Since OTC ear drops and oil contain antibiotics and steroids to treat outer ear infections like swimmer’s ear, they can be used to soften and remove earwax.
Decongestants
- Decongestants can assist to ease congestion and lessen fluid buildup in the middle ear, a common example is pseudoephedrine.
Surgery
- Surgery may be performed to repair a perforated eardrum, remove sick tissue, or place ear tubes to drain fluid from the middle ear.
Home remedies

Home remedies to ease ear infections
In addition to therapies, a number of at-home remedies and self-care techniques can assist in easing the signs and symptoms of an ear infection. These include:
- Applying a warm compress to the afflicted ear to ease discomfort and lessen swelling.
- Resting and refraining from actions that can make the symptoms worse.8Home remedies | Researched based study from Entcolumbia.org
- Maintaining the affected ear in a higher posture results in less pressure inside the ear, which lessens discomfort and swelling.
- Reducing exposure to irritants like chemical smells and cigarette smoke
- Exercises like stretching the neck can also help with earaches.
- Anti-inflammatory herbs like consumption of Ginger also ease discomfort.
Prevention
Preventive Measures for Ear Infection:
By taking preventive measures, one can reduce the risk of developing an ear infection and promote overall ear health. These include:
Good hygiene
- Frequently wash your hands before touching your face or eating. This may aid in halting the spread of pathogens that can result in ear infections.
Avoid smoking
- Ear infections are more likely to occur when smoking since it irritates the lining of the respiratory tract.9Prevention | Researched based study from Nhsinform.scot
Avoid sharing belongings
- The chance of ear infections spreading increases when people share personal objects like towels, earbuds, or headphones.
Get vaccinated
- Infections that lead to ear infections, such as pneumococcal infections and influenza, can be prevented by vaccinations.
Avoid exposure to loud noise
- In noisy areas, wear ear protection like earplugs or noise-canceling headphones.
Diagnosis
Diagnosis for Ear Infection
A doctor or ENT expert will often make the diagnosis of an ear infection. The steps involved in diagnosing ear infections are as follows:
Medical history
- The doctor will inquire about the patient’s symptoms and medical background, especially any prior ear infections.
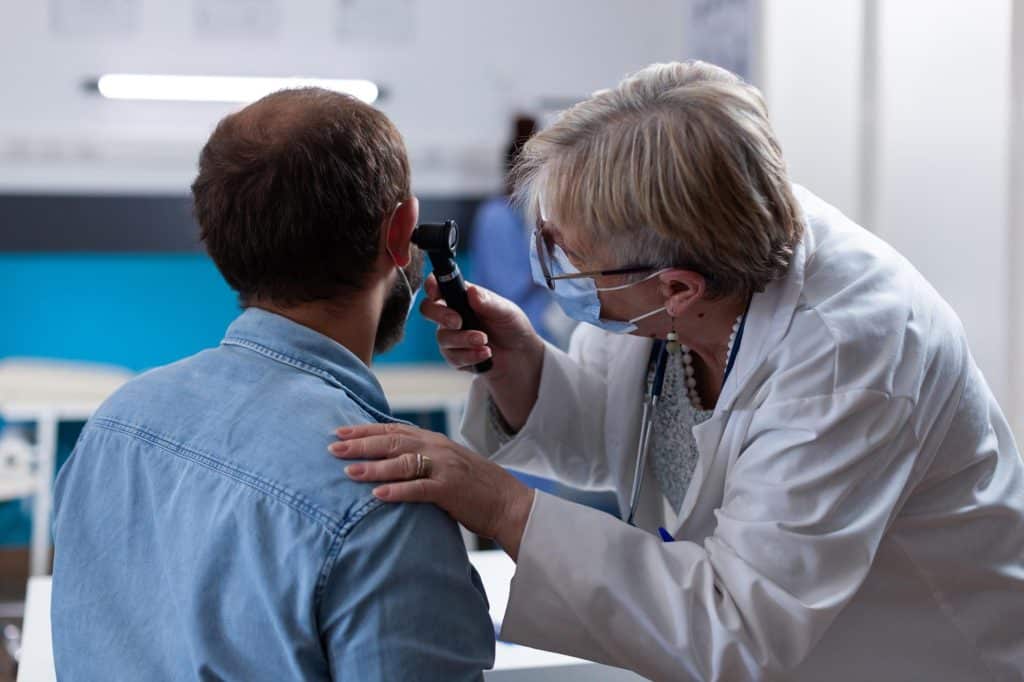
Physical examination
- Using a lighted device known as an otoscope, the healthcare provider will check the patient’s ENT.
- This will enable the doctor to look for indications of inflammation and fluid buildup surrounding lymph nodes and their nearby locations.10Diagnosis | Researched based study from Mountsinai.org
Tympanometry
- In this test, a tool is used to gauge how the eardrum moves in response to variations in air pressure. This can assist in figuring out if there is fluid accumulation in the middle ear.
Audiometry
- This test includes utilizing earphones and a computer to degree the patient’s hearing capacity which makes a difference to recognize any hearing loss.
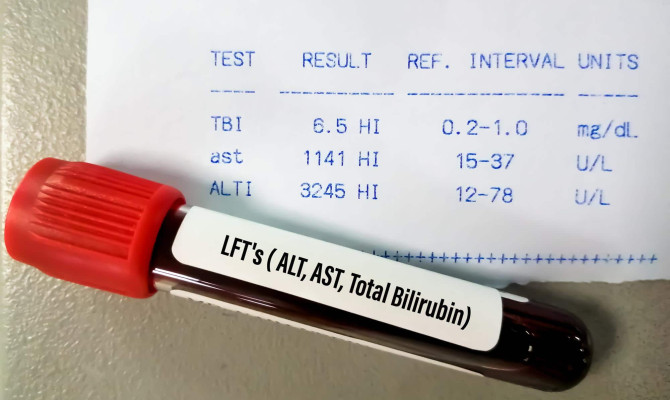
Culture or affectability testing
- If specialist suspects the ear disease is caused by microbes, they may take a test of it and send it for testing which can offer assistance to recognize particular microscopic organisms causing the infection.
Imaging tests
- In a few cases, the specialist may arrange imaging tests such as a CT check or MRI to distinguish any anomalies which will be causing the ear infection.
Side effects
After side-effects of getting treatment
Treatment for ear diseases is by and large secure and viable, but there are a few potential side impacts that patients may encounter. A few common side impacts of treatment are:
Antibiotics
- Anti-microbials are secure but in some cases can cause side impacts like sickness, heaving, runs, unfavorably susceptible responses, or can disturb the adjustment of microscopic organisms within the gut.
Pain relievers
- Taking OTC relievers like acetaminophen or ibuprofen are utilized to diminish torment related to ear diseases which are secure but can cause side impacts like stomach disturbed, and headaches.
Ear drops
- Ear drops containing anti-microbial or steroids may be utilized to treat certain sorts of ear diseases but cause side impacts like itching, burning, or stinging within the ear, as well as brief hearing loss.
Surgery
- In a few cases, surgery may be vital to treat complications which is for the most part secure, but can cause side impacts such as torment, death, or infection.
Complications
What are the complications of not getting ear infection treated
If the infection is left untreated ear disease can cause a run of complications and more well-being issues. A few potential results of untreated ear infections include:
Hearing loss
- Ear contaminations can cause temporary/permanent hearing loss because of the irritation and liquid buildup within the center ear causing harm to the fragile structures of the ear.
Speech delays
- There can be a chance of loss of hearing which can make it troublesome for an individual to hear and understand the dialect, which can affect their capacity to memorize and communicate.
Tympanic membrane puncturing
- In case the weight from the liquid buildup gets to be as well extraordinary, it can cause the eardrum (Tympanic membrane) to burst which can be painful.
Mastoiditis
- When contamination spreads from the center ear to the mastoid bone, it can cause swelling, which can lead to facial loss of motion or meningitis. 6Contamination| Researched based study from Pennmedicine.org
Chronic ear contaminations
- If ear diseases are cleared out untreated, they can become unremitting or repetitive, which can cause drainage from the ear.
Prognosis
Prognosis of ear infections
- The prognosis for ear infections depends on the severity and type of infection. Acute otitis media, caused by a bacterial virus and pus behind the eardrum, generally has a good prognosis if treated promptly.
- Antibiotics are often prescribed to clear the infection; symptoms usually improve within a few days. However, untreated or severe cases can lead to complications such as hearing loss and tympanic membrane rupture.
- Chronic otitis media is caused by inflammation of the middle ear and accumulation of fluid over three months or longer and can have a more difficult prognosis.
- Antibiotics may not be effective in treating chronic otitis media because the problem is not always caused by an infection. Treatment options include surgery to remove fluid and repair damaged eardrums.
- Overall, early diagnosis and treatment are key to a good prognosis for ear infections. If symptoms persist or worsen, or if there are signs of complications, it is important to see a doctor.
Any feedback on this article?
 This Articles content was accurate
This Articles content was accurate Very Informative Article
Very Informative Article I have a question or a comment
I have a question or a comment
 This article contains inaccurate content
This article contains inaccurate content This article was not helpful
This article was not helpful I have a question or a comment
I have a question or a comment
We appreciate your helpful feedback!
Checkout our social pages
References
-
Nationwide Children’s Hospital
Ear Infections (Otitis Media) | Types
-
Better Health Channel
Ear infections | Types
-
Medline Plus
Petrositis | Types
-
Cleveland Clinic
Labyrinthitis | Types
-
Cleveland Clinic
Swimmer's Ear (Otitis Externa) | Causes
-
Penn Medicine
Ear Infection (Otitis) | Causes | Complications
-
Mayo Clinic
Ear infection (middle ear) | Symptoms
-
Columbia University
Otitis Media (Middle Ear Infection) in Adults | Treatment
-
NHS inform
Middle ear infection (otitis media) | Prevention
-
Mount Sinai
Ear infections-Otitis media | Diagnosis