Jaundice: Types, Causes, and Treatment

- Jaundice
- 17 Aug 2023
Overview
What is Jaundice?
Jaundice is a medical condition marked by skin, eyes, and mucous membranes yellowing. Jaundice is a medical word taken from the French word jaune, which means yellow. It is a symptom, not a sickness, of a problem that affects the red blood cells, liver, or gallbladder. Jaundice can affect individuals of all ages, from newborns to the elderly, and understanding its causes, symptoms, and treatment is crucial for timely intervention and management.
This article will delve into the various aspects of jaundice, shedding light on its causes, symptoms, diagnosis, and available treatment options.
Symptoms

Jaundice symptoms
The symptoms of jaundice commonly include:
- Yellow skin
- The yellow sclera of the eyes (Whites)
- Yellowing of mucous membranes.
- Feeling of unwell
- Abdominal pain
- Dark Urine
- Pale stools
- Fatigue
- Weakness
- Itching
- Fever 1Symptoms| Researched based study from Clevelandclinic.org
- Chills
- Joint pain
Types
Types of Jaundice
Jaundice can be of the following types:
- Pre-hepatic
- Hepatic
- Post-hepatic
- Neonatal
Pre-hepatic jaundice
- It happens before the blood reaches the liver.
- Causes unconjugated bilirubin levels to rise2Types| Researched based study from Nlm.nih.gov
Hepatic jaundice
- This happens when the liver’s capacity to remove bilirubin from the blood declines.
- Causes greater levels of both conjugated and unconjugated bilirubin.
Post-hepatic jaundice
- Higher amounts of conjugated bilirubin develop when bilirubin is eliminated in the liver but cannot leave the body due to a blockage.
Neonatal jaundice
- This happens as a result of high total serum bilirubin (TSB) 3Types| Researched based study from Nlm.nih.gov
- Jaundice in newborns is frequent and typically not harmful when treated.
Causes
Jaundice causes
The main cause of jaundice is problems with the liver, gallbladder, or red blood cells, which result in an excess of bilirubin (a yellow pigment) in the blood.
Among the frequent causes of jaundice are
- Liver Diseases – Hepatitis, cirrhosis, alcoholic liver disease, and liver cancer can impair liver function, causing jaundice.
- Gallstones – can prevent the bile from flowing normally via the bile ducts, which can result in jaundice.
- Hemolytic Anemia – In conditions like thalassemia, sickle cell anemia, or autoimmune hemolytic anemia,4Causes| Researched based study from Hopkinsmedicine.org there is an increased destruction of red blood cells, resulting in excessive bilirubin production.
- Biliary Tract Disorders – Conditions like biliary atresia, primary biliary cirrhosis, and primary sclerosing cholangitis can obstruct the bile ducts and cause jaundice.
- Pancreatic disorders – like pancreatic cancer or pancreatitis, can interfere with the production and release of digestive enzymes and bile, resulting in jaundice5Causes| Researched based study from Mayoclinic.org
- Medications – like certain antibiotics, acetaminophen, and nonsteroidal anti-inflammatory drugs (NSAIDs), can cause liver damage and jaundice in rare cases.
Risk factors
Risk factors of Jaundice
The following are the risk factors for jaundice:
- Genetic conditions – inherited disorders like Dubin-Johnson and Gilbert’s syndrome can increase the risk2Risk| Researched based study from Nlm.nih.gov
- Pregnancy difficulties like premature birth and Rh incompatibility 6Risk| Researched based study from Medlineplus.gov between the mother and baby can increase the risk and severity of newborn jaundice.
- Age – Newborns are more susceptible to jaundice. Older adults may also be at a higher risk due to a higher prevalence of liver diseases.
- An unhealthy diet rich in saturated fats, refined sugar, and processed food can contribute to obesity and non-alcoholic fatty liver disease (NAFLD), leading to jaundice.7Risk| Researched based study from Mayoclinic.org
- Medicines – certain medicines like NSAIDs (Nonsteroidal anti-inflammatory drugs) and steroids can cause liver injury and lead to jaundice.
- Alcohol or substance abuse – excessive alcohol consumption 8Risk| Researched based study from Nlm.nih.gov or substance abuse can lead to liver damage and increases the risk of jaundice.
- Environmental factor – exposure to toxins like certain chemicals, pollutants, etc., can result in jaundice.
- Unprotected sex – increases the risk of contracting viral infections like hepatitis B or C, which can cause liver damage and jaundice.
Diagnosis
Diagnosis of Jaundice
The doctor arrives at a diagnosis of jaundice after a thorough medical history and physical examination, followed by a few tests as follows:
Physical examination
The doctor may
- Look for yellow discoloration of the skin, sclera, and oral mucosa.
- Check for skin bruising.
- Checks for fever with the help of a thermometer.
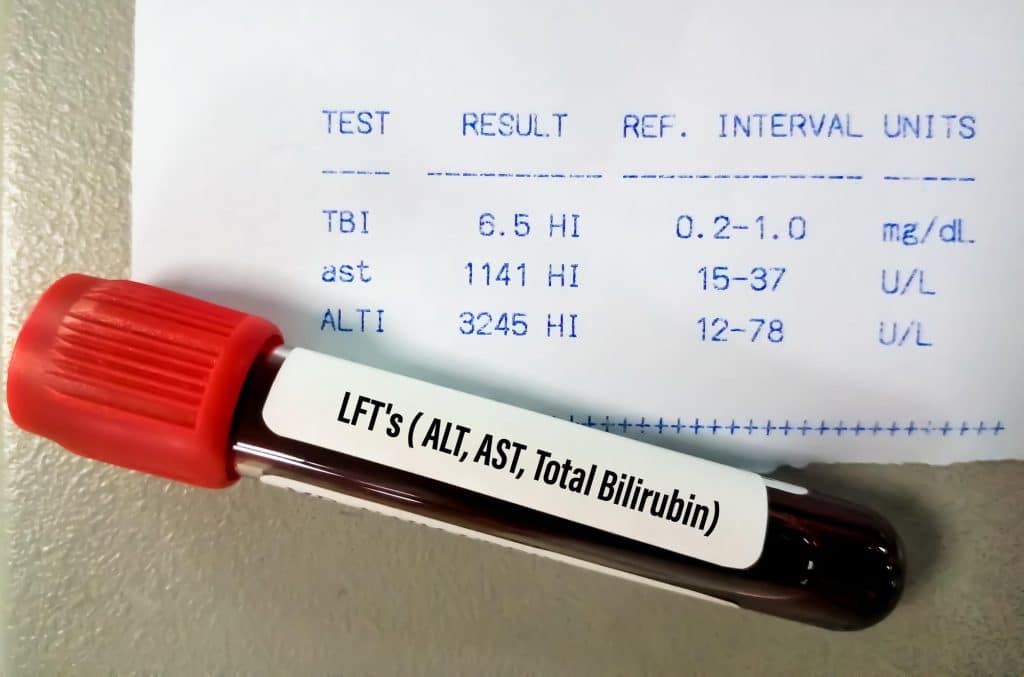
Laboratory tests
- Blood Tests – including Complete blood count (CBC), liver function tests, etc. can measure the number of blood cells available, levels of bilirubin in the blood, and liver enzymes to identify the potential causes.
- Imaging Tests – Ultrasound, CT, or MRI scans can help visualize the liver, gallbladder, and bile ducts to detect abnormalities.
- Liver Biopsy – In some instances, a liver biopsy may be required to examine liver tissue and determine the cause of jaundice9Diagnosis| Researched based study from Mountsinai.org
Treatment
How is Jaundice treated?
Effective management and treatment of jaundice can be achieved if the cause has been found.
Some common treatment approaches include:
Managing Liver Diseases
- Through lifestyle modifications, drugs to control symptoms and delay the disease’s progression, and, in severe circumstances, liver transplantation.
Treating Hemolytic Anemia
- Focuses on treating the underlying condition. This may include blood transfusions, medications to suppress the immune system, and folic acid supplementation.
Treating Biliary Tract Disorders
- It depends on the specific condition but may involve medications to improve bile flow.
Medication Adjustments
- It may be required if drugs are causing jaundice. The medical professional may change the dosage, use different medications, or stop prescribing the prescription altogether.
Surgical management
- It may be needed to treat jaundice if the underlying cause is bile duct obstruction, liver failure, gall stone, pancreatic cancer, or extensive and permanent liver damage10Diagnosis| Researched based study from Healthdirect.gov
In addition to treating the underlying cause, symptomatic relief measures may alleviate discomfort associated with jaundice. These may include:
Itching Relief
- Antihistamines or medications specifically prescribed for itching, such as cholestyramine, may alleviate itchiness.2Treatment| Researched based study from Nlm.nih.gov
Fluid and Electrolyte Balance
- In cases of dehydration or electrolyte imbalances, intravenous fluids may be administered to restore balance.
Nutritional Support
- A balanced diet, including adequate protein and calories, is essential for individuals with jaundice. In some cases, dietary supplements may be recommended.
Food to avoid during jaundice
- Refined carbohydrates like refined sugar, white bread, packaged or canned food, and meat like beef or pork as they can lead to strain of liver, raw or undercooked fish, or shellfish.
Prevention
Prevention of Jaundice
Even while specific causes of jaundice cannot be avoided, some steps may be taken to reduce the risk of some disorders, such as:
- Hepatitis A and B vaccination can drastically lower the risk of liver infections and subsequent jaundice.
- Liver infections and jaundice can be avoided by utilizing safe behaviors, such as safe sex and clean needles.
- Refrain from ingesting too much alcohol.
- Regular exercise and a healthy diet may make weight and cholesterol levels easier.
- Regular checkups can help in the early discovery of liver problems, allowing for prompt management and intervention.
Complications
Complications of Jaundice
Depending on the underlying etiology, there may be different jaundice complications.
Kernicterus
- Kernicterus, also known as bilirubin encephalopathy, can result from jaundice, especially in newborns
- In which indirect or unconjugated bilirubin at high concentrations harms the brain and neurological system and can cause lasting damage11Complications| Researched based study from Nlm.nih.gov
Outlook
The Outlook
The prognosis of jaundice varies depending on the underlying cause. Jaundice must be diagnosed and treated as soon as possible to be effectively managed. Individuals with jaundice can obtain the appropriate care to address the underlying problem and alleviate accompanying symptoms if they understand the causes, recognize the signs, and seek timely medical help.
Any feedback on this article?
 This Articles content was accurate
This Articles content was accurate Very Informative Article
Very Informative Article I have a question or a comment
I have a question or a comment
 This article contains inaccurate content
This article contains inaccurate content This article was not helpful
This article was not helpful I have a question or a comment
I have a question or a comment
We appreciate your helpful feedback!
Checkout our social pages
References
-
Cleveland Clinic
Adult Jaundice | Symptoms
-
National Library of Medicine
Jaundice | Types
-
National Library of Medicine
Neonatal Jaundice | Types
-
Johns Hopkins Medicine
Hemolytic Anemia | Causes
-
Mayo Clinic
Pancreatic cancer | Causes
-
Medline Plus
Rh incompatibility | Risk
-
Mayo Clinic
Nonalcoholic fatty liver disease | Risk
-
National Library of Medicine
Alcoholic Hepatitis | Risk
-
Mount Sinai
Jaundice | Diagnosis
-
Health Direct
Jaundice in adults | Treatment
-
National Library of Medicine
Kernicterus | Complications