Cervical cancer and its management

- Cervical Cancer
- 22 Aug 2023
Overview
What is Cervical cancer ?
A type of cancer that originates in the cervix is called cervical cancer. The uterus’s lowest point, which connects to the vagina, is known as the cervix. Cervical cancer is the world’s fourth most prevalent malignancy among women. 1Overview| Researched based study from Nlm.nih.gov Most cervical cancers are due to sexually transmitted human papillomavirus strains (HPV). When encountering HPV, the body’s defense mechanism prevents the virus from causing harm. However, in a small number of people, the virus remains for years, converting some cervical cells into cancer cells. By getting screened and vaccinated against HPV infection, one can lower their risk of contracting the disease.
Causes
Causes of cervical cancer
- Although the exact cause of cervical cancer is unknown, the sexually transmitted HPV virus is undoubtedly a factor. About half of all cervical pre-cancers are caused by the Human Papillomavirus (HPV) strains 16 and 18. 2Causes | Researched based study from Who.int
- Cancer-causing HPV can spread through sexual activity, either anal, vaginal or oral.
- Most people who carry the virus never develop cancer, suggesting that other elements, such as one’s environment or lifestyle choices, also have a role in determining a person’s risk of developing cervical cancer.
Symptoms
Symptoms of Cervical Cancer
Early stage symptoms
In its early stages, cervical cancer typically exhibits no symptoms, making it challenging to identify. When cervical cancer in its early stages does manifest symptoms, these may include:3Symptoms | Researched based study from Cancer.gov
- Bleeding after having intercourse.
- Bleeding or spotting following menopause.
- Bleeding between periods, heavy periods, or periods that last longer than usual.
- Increased vaginal discharge that occasionally smells bad and may contain blood.
- Light bleeding or irregular spotting between cycles in females of reproductive age.
- Pelvic pain or discomfort during intercourse.
Advanced Symptoms
Advanced cervical cancer symptoms might include early-stage cervical cancer symptoms as well as the following:3Symptoms | Researched based study from Cancer.gov
- Swollen legs.
- Abdominal ache.
- Being exhausted.
- Ongoing leg, pelvic, or back pain.
- Appetite loss, exhaustion, and weight loss.
- Blood in the urine, painful or difficult urination.
- Uncomfortable or painful bowel movements.
- Rectum bleeding during a bowel movement.
Risk
Risk factors
Cervical cancer risk factors include:
A weakened immune system
- Immunocompromised individuals have a higher risk of HPV infections persisting and developing into cancer.
- Examples include HIV patients, transplant recipients on immunosuppressants, and people with autoimmune diseases.
Multiple partners
A person has a higher risk of contracting HPV if they have more sexual partners overall, as well as if their partners have multiple sexual partners.4Risk | Researched based study from Mayoclinic.org
Early sexual activity
Having intercourse at a younger age increases one’s risk of HPV.
Other STIs (sexually transmitted illnesses)
- Co-occurring STIs such as gonorrhoea, chlamydia, syphilis and HIV/AIDS increase the risk.
Smoking
- The chance of acquiring cervical cancer of the squamous cell type is higher in people who smoke or breathe in secondhand smoke.4Risk | Researched based study from Mayoclinic.org
Other reproductive factors
- Cervical cancer risk is linked with consuming contraceptives and having several children. These associations’ causes are not entirely clear.
Exposure to a medication
- Diethylstilbestrol (DES) use during pregnancy in the 1950s may have elevated the chance of clear cell adenocarcinoma, a specific type of cervical cancer, in a person’s offspring.4Risk | Researched based study from Mayoclinic.org
Prevention
Preventing cervical cancer
The following may help prevent cervical cancer in an individual:
- When having sex, put up a barrier like a condom.
- Try to limit sexual partners.
- Vaccinate against HPV – for both sexes, aged 9 to 45, the FDA has approved Gardasil-9. It offers defence against several HPV strains. 5Prevention| Researched based study from Fda.gov
- Giving up smoking – may lower the chance of developing cervical cancer.
- PAP and HPV testing – Every five years, people between the ages of 25 and 65 should undergo an HPV and PAP test. If the doctor determines that the patient is at low risk after that age, they may be allowed to quit testing.
- Performing an STD screening – Sexually active people may benefit from yearly testing for various STDs such as gonorrhoea, chlamydia, HIV, and syphilis.
- Consume a healthy balanced diet to improve the immune system’s performance.
Diagnosis
Diagnosis of cervical cancer
Diagnosis of cervical cancer may include screening, biopsy and staging.
Screening
Screening tests may aid in finding precancerous cells that could one day turn into cervical cancer. The majority of guidelines recommend starting cervical cancer screenings at age 21.
Screening exams consist of:
PAP test or PAP smear
- Identifies unhealthy or irregular cells in the cervix.
HPV test
- Finds the high-risk HPV infection subtypes most likely to result in cervical cancer. 6Screening| Researched based study from Cancer.gov
Additional testing may be necessary if screening tests reveal an HPV infection:
Biopsy
- If the doctor suspects cancer, they may check the patient’s cervix and collect a tissue sample for a biopsy.
- The doctor can obtain tissues via various methods, including punch biopsy, a wire loop, endocervical curettage, and conization.
- If the biopsy finds cancer, additional tests will reveal whether the condition has spread.
Further tests may include:
- Liver function test.
- Kidney function test.
- Blood and urine analysis.
- Imaging tests of the bladder, intestines, rectum and abdominal cavity. (X-rays, CT scan, ultrasound, or MRI)
Stages
Stages of cervical cancer
- Stage I – Cancer restricted within the cervix, has not spread and is mild.
- Stage II – has progressed past the uterus and cervix but hasn’t yet reached the vagina or pelvic wall.
- Stage III – has progressed to the lower vagina and might also have affected the ureters, pelvic wall, and adjacent lymph nodes.
- Stage IV – has progressed to the rectum, bladder, or other organs or body components, such as the bones or lungs. 7Stages | Researched based study from Clevelandclinic.org
Treatment
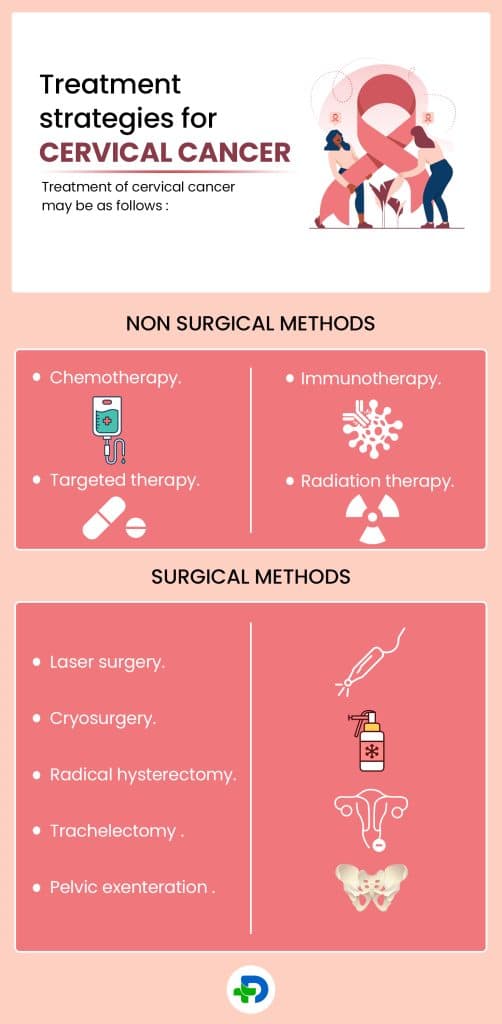
Treatment strategies
Treatment of cervical cancer may be as follows:
Non surgical methods
- Treatment of precancerous lesions – The doctor could remove a low-grade lesion if it is present during a biopsy.
- Chemotherapy – uses potent drugs to battle cancer cells. Doctors widely prescribe it for the internal or localized spread of cervical cancer.
- Targeted therapy – concentrates on particular flaws in cancer cells. Targeted pharmacological treatments can kill cancer cells by sabotaging these flaws. For cervical cancer is advanced, it can be a possibility.
- Immunotherapy –encourages the immune system activity with medication to find and eliminate cancer cells. It also makes it possible for cancer cells to avoid deceiving the body into believing they are healthy cells.
- Radiation therapy – destroying cancer with high-energy radiation (like X-rays)8Treatment | Researched based study from Cdc.gov Both options include radiation therapy with an external beam or brachytherapy.
- Supportive palliative care – The goal is to enhance cancer patients’ quality of life. The supportive palliative care team provides this type of care and other treatments.
Surgical methods
If the cancer is tiny and non-invasive, it can be eliminated by
- Laser surgery – the surgeon employs a laser beam to destroy cancer cells.
- Cryosurgery – aids in freezing cancer cells.
For invasive types, the following techniques may be used:
- A simple hysterectomy removes the uterus without removing the tissue around it. Nodes in the pelvis and vagina are left in place.
- Radical hysterectomy – The uterus, the cervix, a tiny bit of the upper vagina, the parametrium (the tissue surrounding the uterus), and pelvic lymph nodes are all removed. 9Treatment | Researched based study from Cancer.org
- Trachelectomy – The cervix & the upper portion of the vagina are removed, but the uterus is left behind.
- Pelvic exenteration – Similar to a radical hysterectomy, but depending on how far the cancer has gone, it may also remove part of the colon, the bladder, the vagina, and the rectum.
Complications
Complications of cervical cancer
Cervical cancer complications can include:
- Recurrence – women receiving treatment to save their uterus are at risk for cancer to recur.
- Issues with bowel and bladder.
- Limited sexual function following treatment with radiation or surgery.
- After uterine removal, they are unable to get pregnant.
- Cancer spreads to other body parts like bone, the spinal cord or the brain.
- Kidney failure.
- Bleeding.
Care
How to provide care ?
An official diagnosis of cervical cancer will be challenging to deal with. However, one might attempt the following to cope with the situation:
- Educating oneself on cervical cancer may aid in helping a patient choose the right course of treatment.
- Find someone to talk to; one may feel better by venting to friends or relatives. People in similar situations can speak to each other by joining support groups.
- Consume a balanced diet. According to the advice of your doctor or a nutritionist, eat various fruits and vegetables.
- Discover relaxation strategies, including mindfulness exercises, meditation, yoga, regular exercise, and time spent with family, friends, or pets.
- Get adequate sleep – the body needs it for healthy immunological function. Furthermore, getting enough sleep may lessen stress.
- Accept assistance from others and let loved ones know how they may help.
- Set manageable goals – feeling in control and having a sense of direction are enhanced by having minor goals.
- If a person is feeling depressed or nervous about the situation, seek assistance from a mental health professional or a counsellor.
Outlook
Outlook
Primary prevention and screening are the most successful strategies for reducing cervical cancer-related mortality. A cost-effective method of preventing cervical cancer is HPV vaccination, pre-cancer lesion screening, and treatment. When monitored and carefully treated, the doctor can cure precancerous diseases. The factors determining an individual’s prognosis with cervical cancer are the type of cancer, the extent to which it has spread, the individual’s age and general health, and whether or not the cancer returns after therapy.
Any feedback on this article?
 This Articles content was accurate
This Articles content was accurate Very Informative Article
Very Informative Article I have a question or a comment
I have a question or a comment
 This article contains inaccurate content
This article contains inaccurate content This article was not helpful
This article was not helpful I have a question or a comment
I have a question or a comment
We appreciate your helpful feedback!
Checkout our social pages
References
-
National Library of Medicine
Cervical Cancer | Overview
-
World Health Organization
Cervical cancer-factsheet | Causes
-
National Cancer Institute
Cervical Cancer | Symptoms
-
Mayo Clinic
Cervical Cancer | Risk
-
U.S Food and Drug Administration
GARDASIL 9 | Prevention
-
National Cancer Institute
Cervical cancer | Screening
-
Cleveland Clinic
Cervical Cancer | Stages
-
Centers for Disease Control and Prevention
How Is Cervical Cancer Diagnosed and Treated? | Treatment
-
American Cancer Society
Surgery for Cervical Cancer | Treatment