Pelvic inflammatory disease: Types, Causes and Treatment

- Pelvic Inflammatory Disease (PID)
- 22 Aug 2023
Overview
What is Pelvic inflammatory disease?
Pelvic inflammatory disease (PID) is a female reproductive organ infection that may affect the ovaries, fallopian tubes, and the uterus. PID, if not treated promptly, could lead to severe complications and long-term harm to the reproductive system.
This article will explore the symptoms, types, causes, risk factors, diagnosis, treatment, prevention, complications, and prognosis associated with pelvic inflammatory disease.
Symptoms

Symptoms of PID
The common symptoms of Pelvic inflammatory disease (PID) may include:
- Abdominal pain
- Irregular menstrual bleeding
- Abnormal vaginal discharge 1Symptoms| Researched based study from Clevelandclinic.org
- Painful urination
- Painful sexual intercourse
- Fever and fatigue
Abdominal pain
- Women with PID commonly experience mild to severe lower abdominal pain.
- The feeling of pain might be dull, continuous, or irregular, and it can get worse during menstruation or sexual intercourse.
Irregular menstrual bleeding
- PID can cause irregular or heavier-than-usual menstrual bleeding.
Abnormal vaginal discharge
- A change in vaginal discharge is another common symptom of PID.
- The discharge may be yellow or greenish and may have an unpleasant odor.
Painful urination
- A burning or painful sensation during urination is possible in some patients.
Painful sexual intercourse
- During sexual intercourse, PID can result in discomfort or pain. 1Symptoms| Researched based study from Clevelandclinic.org
Fever and fatigue
- Women with severe PID may experience fever, tiredness, nausea, and overall malaise.
Types
Types of Pelvic inflammatory disease
There are two primary types of PID:
- Acute PID – is a sudden and severe infection of the reproductive organs.2Types| Researched based study from Nlm.nih.gov
- Chronic PID – is a prolonged inflammation of the female reproductive system caused by repeated or untreated acute PID and can lead to various consequences.
Causes
Causes of Pelvic inflammatory disease
- It is typically due to sexually transmitted infection, where the bacterial infection travels from the cervix into the upper reproductive organs, resulting in inflammation and infection.
- Various bacteria can cause PID, but the two most prevalent diseases are gonorrhea and chlamydia.2Causes| Researched based study from Nlm.nih.gov
- Mycoplasma genitalium, a cervical bacterium, can also cause it.
- PID can also be caused by non-sexual illnesses such as a ruptured appendix, intestinal infections such as gastroenteritis, or surgical operations such as abortion, ectopic pregnancy, childbirth, or insertion of an intrauterine device.3Causes| Researched based study from Betterhealth.vic.gov.au
Risk factors
Pelvic inflammatory disease risk factors
Several factors can increase a woman’s risk, including:
- Age
- Unprotected sexual activity
- Multiple partners
- History of STIs
- Intrauterine devices (IUD)
- Recent pelvic surgery
- Douching
Age
- Women under 25 who engage in sexual activity are more vulnerable than others.4Risk factors| Researched based study from Cdc.gov
Unprotected sexual activity
- PID risk is increased by unprotected sexual activity and having several sexual partners.
Multiple partners
- Having several sexual partners or having a sexual connection with an individual with more than one.
History of STIs
- PID is more likely in people who have a history of sexually transmitted illnesses like gonorrhea or chlamydia.
Intrauterine device (IUD) use
- Despite being uncommon, the risk of PID increases slightly shortly after the placement of an intrauterine device and may be limited to the first few weeks following insertion.4Risk factors| Researched based study from Cdc.gov
Recent pelvic surgery
- Women who have undergone recent pelvic surgery, such as abortion or hysterectomy, are at an increased risk of developing PID.5Risk factors| Researched based study from Nlm.nih.gov
Douching
- Regular use of vaginal douches can raise the risk of PID by upsetting the normal balance of bacteria in the vagina.6Risk factors| Researched based study from Nlm.nih.gov
Diagnosis
Diagnosis of Pelvic inflammatory disease
Prompt and accurate diagnosis of PID is crucial for effective treatment. The diagnostic process may involve:
- Medical history – Doctor will inquire about symptoms, sexual history, contraceptive methods used, and recent pelvic procedures.
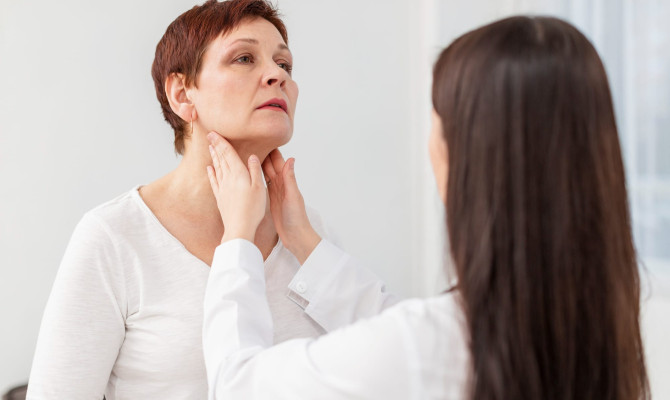
- A pelvic examination – to check for any abnormal discharge, tenderness, or swelling of the reproductive organs.
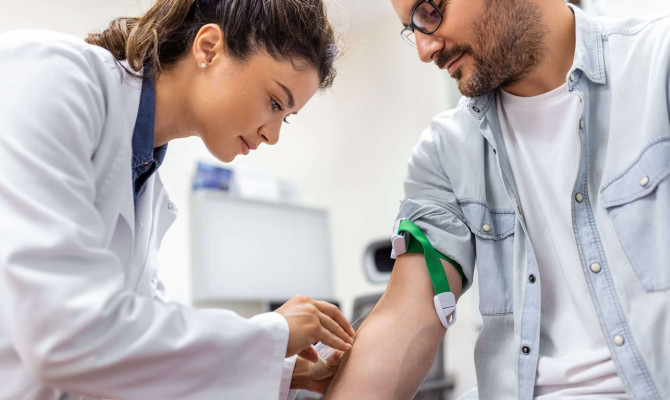
- Blood and urine test – to screen for sexually transmitted infections (STDs) and inflammation.
- Pap test – Cells from the cervix are taken out for this test and inspected under the microscope for cells that are cancerous, infections, or inflammations.7Diagnosis| Researched based study from Hopkinsmedicine.org
- Imaging tests – Ultrasound or other imaging techniques may be used to visualize the reproductive organs and identify abnormalities.
- Biopsy – a small portion of endometrial tissue is removed and tested for signs of infection and inflammation.8Diagnosis| Researched based study from Acog.org
Treatment
Treatment of Pelvic inflammatory disease
Pelvic inflammatory disease treatments typically involve:
- Oral antibiotics – Depending on the type of infection, the bacteria that may be present or suspected, and the particular patient’s circumstances, oral antibiotics may be recommended. Even if symptoms subside, finishing the entire antibiotic course is vital to guarantee the illness is completely cured.
- Hospitalization – required mainly in cases of severe PID, complications, or ineffective oral antibiotics. Intravenous antibiotics (given through veins) and thorough monitoring may be used in hospital-based treatment.
- Treatment for a partner – To prevent re-infection, the woman’s sex partner should also be treated. This is because they may still be carriers of the infection despite not showing any symptoms.9Treatment| Researched based study from Cdc.gov
- Avoid sexual activity – until treatment is finished and symptoms have disappeared.10Treatment| Researched based study from Mayoclinic.org
- Surgery – may be required if a woman’s symptoms persist or an abscess fails to heal.9Treatment| Researched based study from Cdc.gov
Prevention
Prevention of Pelvic inflammatory disease
Following are some of the preventive measures to reduce a person’s risk:
- Practice safe sex – Use condoms consistently and maintain a relationship that is mutually monogamous to help lower the possibility of STIs that contribute to PID.11Prevention| Researched based study from Mayoclinic.org
- Regular STI testing – Get tested for STIs on a regular basis, especially if you participate in high-risk sexual activities or have several partners.
- Get prompt treatment of STIs – If diagnosed with an STI, seek timely treatment and ensure that your sexual partners are tested and treated.
- Do not Douch – as it can upset the vaginal bacteria’s normal equilibrium, raising the risk of infection.12Prevention| Researched based study from Plannedparenthood.org
- Be cautious with intrauterine devices (IUDs) – people who choose to use an IUD, should ensure it is inserted by a healthcare professional following proper sterile techniques. Attend regular check-ups to monitor the device’s placement and promptly address any concerns.
Complications
Complications of Pelvic inflammatory disease
Recurrent or untreated PID can lead to several complications including:
- Ectopic pregnancy
- Infertility
- Tubo-ovarian abscess (TOA)
- Chronic pain
Ectopic pregnancy
- Scarring and fallopian tube damage raise the likelihood of ectopic pregnancies, in which the eggs that are fertilized gets implanted outside of the uterus.
- Ectopic pregnancies are risky and must be treated immediately.13Complications| Researched based study from Healthdirect.gov
Infertility
- PID can damage and scar the reproductive organs, especially the fallopian tubes which can result in blocked or damaged tubes, leading to difficulties in conceiving.
Tubo-ovarian abscess
- A pelvic inflammatory disease can cause an infectious mass in the reproductive system. 14Complications| Researched based study from Nlm.nih.gov
Chronic pelvic pain
- Some patients may have persistent pelvic pain even after the infection has cleared.
- Chronic pelvic pain can have an important effect on everyday living and may necessitate continuing therapy.
Prognosis
Prognosis of Pelvic inflammatory disease
PID has a typically favorable prognosis when diagnosed early and treated appropriately. However, it is essential to complete the entire course of antibiotics and follow up with healthcare providers to ensure a complete resolution of the infection. By promoting safe sex, seeking timely treatment for STIs, and adopting good hygiene practices, the risk of developing PID can be significantly reduced. Early intervention and treatment adherence are key to preventing complications and ensuring a favorable prognosis for individuals affected by PID.
Any feedback on this article?
 This Articles content was accurate
This Articles content was accurate Very Informative Article
Very Informative Article I have a question or a comment
I have a question or a comment
 This article contains inaccurate content
This article contains inaccurate content This article was not helpful
This article was not helpful I have a question or a comment
I have a question or a comment
We appreciate your helpful feedback!
Checkout our social pages
References
-
Cleveland Clinic
Pelvic Inflammatory Disease | Symptoms
-
National Library of Medicine
Pelvic Inflammatory Disease | Types
-
Better health channel
Pelvic inflammatory disease (PID) | Causes
-
Centers for Disease Control and Prevention
Pelvic Inflammatory Disease (PID) – CDC Basic Fact Sheet | Risk factors
-
National Library of Medicine
Development of Pelvic Inflammatory Disease after Ectopic Removal | Risk factors
-
National Library of Medicine
Vaginal douching as a possible risk factor for pelvic inflammatory disease | Risk factors
-
John Hopkins Medicine
Pelvic Inflammatory Disease (PID) | Diagnosis
-
American College of Obstetricians and Gynecologists
Pelvic Inflammatory Disease (PID) | Diagnosis
-
Centers for Disease Control and Prevention
Pelvic Inflammatory Disease (PID) Treatment and Care | Diagnosis
-
Mayo Clinic
Pelvic inflammatory disease (PID) | Diagnosis
-
Mayo Clinic
Pelvic inflammatory disease (PID) | Prevention
-
Planned Parenthood Federation of America
Pelvic Inflammatory Disease (PID) | Prevention
-
Health Direct
Pelvic inflammatory disease | Complications
-
National Library of Medicine
Tubo-Ovarian Abscess | Complications