Understanding Hemodialysis: Types, Process, Benefits and Complications

- Hemodialysis
- 22 Aug 2023
Overview
About Hemodialysis
Healthy kidneys clean your blood, and surplus fluid is eliminated through urine. They also create compounds that are beneficial to your health.1Overview| Researched based study from Medlineplus.gov When the kidneys cease working, dialysis takes up some of these tasks. Hemodialysis is a type of dialysis that successfully filters and purifies the blood of patients whose kidneys are no longer efficiently eliminating waste materials and extra fluids. It aids in preserving the bloodstream’s critical chemical equilibrium, which is necessary for maintaining fluid and electrolyte levels and overall health.
This article discusses what hemodialysis is, how it works, various types of hemodialysis, its indications, contraindications, advantages, downsides, and limitations.
Types
Types of Hemodialysis
There are two primary types of hemodialysis:
- Conventional In-center hemodialysis
- Home hemodialysis
Conventional In-Center Hemodialysis
- It is the most prevalent type of hemodialysis, in which patients are treated in a dedicated facility.
- The treatment, usually performed three times per week, is overseen by trained medical personnel.
Home Hemodialysis
- Patients can receive hemodialysis treatments at home, where they can do so in comfort.2Types| Researched based study from Kidney.org
- This approach may produce greater results for certain patients because it allows for more scheduling flexibility and can be used more frequently.
- It does call for more training and responsibility on the part of the patient and caregiver.
The Process
How is Hemodialysis performed?
Here is a summary of what happens during a regular hemodialysis session:
- Patient preparation – The patient’s weight, vital signs, and state of health are evaluated when they arrive. Any required changes are made to the prescribed drugs or dialysis schedule.
- Vascular access connection – One needle is used to take blood, and the other is used to return purified blood to the vascular access point, or in the case of a central venous catheter, a catheter.
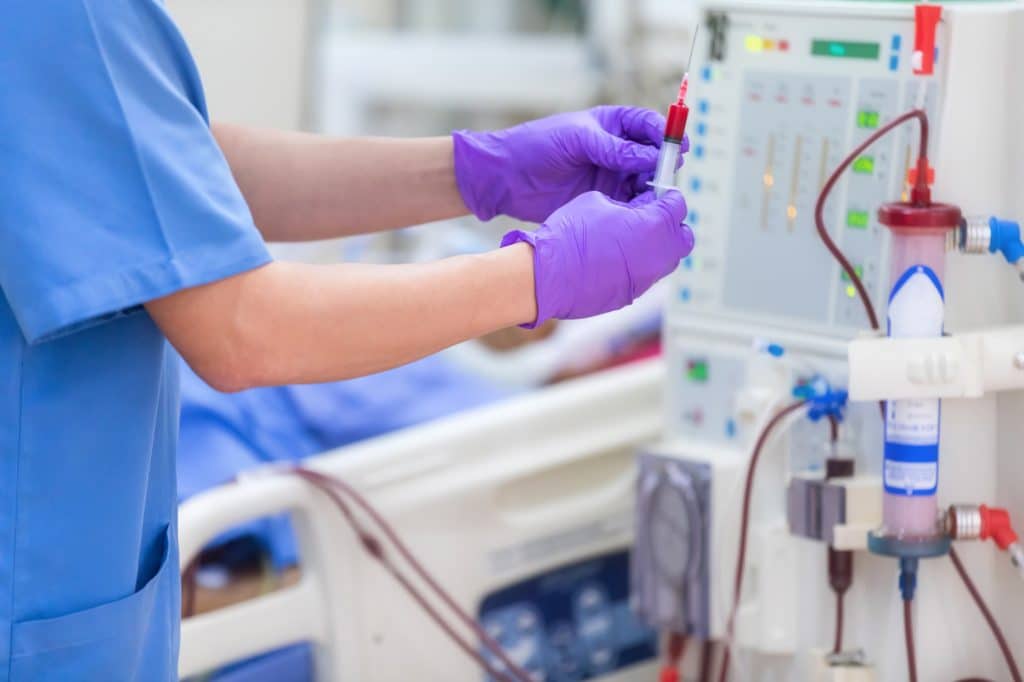
- Blood circulation and filtration – The access site continually pumps the patient’s blood into the hemodialysis machine and out of their body. Before returning to the patient’s bloodstream, the dialyzer inside the machine filters and cleans the blood.3The Process| Researched based study from Nephcure.org
- Monitoring – To guarantee security and efficacy, the patient’s vital signs, like blood pressure, heart rate, and fluid evacuation, are constantly watched throughout the session.6The Process| Researched based study from Mayoclinic.org
- Completion and Recovery – The patient is unplugged from the machine, and the access site is wrapped once the session’s allotted period (usually 3 to 5 hours) has passed. Patients are recommended to relax following the treatment since they can feel weak or exhausted.
Preparations
How to prepare for hemodialysis?
Patients must undergo several preparations before beginning hemodialysis to guarantee a smooth and effective operation. Here are some crucial steps:
- Vascular access placement – An arteriovenous fistula, an arteriovenous graft, or a central venous catheter are typical examples of acceptable vascular access sites that must be created in the first phase. The patient must have access to this to be connected to the hemodialysis machine for each session.4Preparations| Researched based study from Ucsf.edu
- Dietary changes – To ease the strain on their kidneys and maintain greater control during hemodialysis, patients may need to undertake nutritional changes, such as reducing their salt, potassium, and phosphorus consumption.5Preparations| Researched based study from Niddk.nih.gov
- Medication review – Some medications may need to be altered or amended because they can complicate or interfere with the dialysis procedure.
- Scheduling and Regular Appointments – Patients must follow a consistent schedule for their hemodialysis sessions, commonly performed thrice weekly. Serious health repercussions can result from skipping visits.
Uses

Uses of Hemodialysis
The doctor may recommend hemodialysis for the following conditions:
- Chronic kidney failure
- Sudden kidney injury
- Acute renal failure
- Pericarditis 7Uses| Researched based study from Nlm.nih.gov
- End-stage kidney disease (ESKD)
- Poisoning from toxic ingestion
- High levels of potassium in the blood
- Metabolic acidosis
Contraindications
Contraindications
Hemodialysis is not recommended for people with the following conditions:
- Difficult vascular access.
- Heart failure.7Contraindications| Researched based study from Nlm.nih.gov
- Bleeding disorders.
- Needle phobia (fear of needles).
Benefits
Benefits of Hemodialysis
Hemodialysis is a vital technique that offers people with kidney insufficiency a number of benefits:
- Waste product removal – eliminates waste materials and extra fluid from the bloodstream, stopping the accumulation of toxins that can cause life-threatening issues.
- Fluid Balance – Hemodialysis aids in preserving the body’s ideal fluid balance, essential for controlling blood pressure and preventing edema.6Benefits| Researched based study from Mayoclinic.org
- Improved Quality of Life – By successfully controlling renal failure, hemodialysis can enhance patients’ quality of life in general and enable them to carry on with everyday tasks and obligations.
- Accessibility – Many in-center hemodialysis facilities make treatment available to many requiring it.
Disadvantages
Disadvantages and Limitations
Despite being effective, hemodialysis has several drawbacks and restrictions:
- Time-consuming – A patient’s everyday life may be impacted by the three sessions of in-center hemodialysis that are usually needed, each lasting several hours.
- Dietary restrictions – Hemodialysis patients must adhere to stringent nutritional guidelines to adequately manage their condition, which can be complex and constricting.
- Risk of Complications – As with any medical operation, hemodialysis poses potential consequences such as infection, dizziness, nausea, low blood pressure, muscular cramps, skin itching, headaches, chest pain, pain in the back, and entry site difficulties.8Disadvantages| Researched based study from Clevelandclinic.org
- Dependence on Devices – Hemodialysis is difficult for patients in remote locations or with little accessibility to such resources because it primarily depends on modern equipment and healthcare services.
Complications
Complications
Hemodialysis can cause the following complications:
- Low blood pressure 9Complications| Researched based study from Kidney-interantional.org
- Nausea or vomiting
- Muscle cramps
- Abdominal cramps
- Shortness of breath
- Itchy skin
- Problems with sleep
- Body ache
- Restless legs
- Anemia 10Complications| Researched based study from Nlm.nih.gov
- Weak bones
- Infection
- Narrowing of blood vessels
- High potassium levels
- Blocked blood vessels
- Low potassium levels
- Stiffness and fluid in the joints
- Dialysis-related amyloidosis.11Complications| Researched based study from Nlm.nih.gov
- Anxiety or depression
- Heart failure
Bottom line
The Bottom Line
Hemodialysis has changed how end-stage renal illness and chronic kidney failure are managed. It balances necessary components in the bloodstream by efficiently filtering and purifying the blood, enabling patients to live more normally. Despite significant drawbacks and difficulties, it is a vital therapy option for millions worldwide. The benefits of hemodialysis considerably outweigh these limitations and problems. Patients with kidney problems should collaborate with their healthcare providers to develop the best treatment plan and make informed decisions about their long-term health and well-being.
Any feedback on this article?
 This Articles content was accurate
This Articles content was accurate Very Informative Article
Very Informative Article I have a question or a comment
I have a question or a comment
 This article contains inaccurate content
This article contains inaccurate content This article was not helpful
This article was not helpful I have a question or a comment
I have a question or a comment
We appreciate your helpful feedback!
Checkout our social pages
References
-
Medline Plus
Dialysis | Overview
-
National Kidney Foundation
Choosing Dialysis: Which type is right for me? | Types
-
NephCure
Hemodialysis | The Process
-
The Regents of the University of California.
Vascular Access for Hemodialysis | Preparation
-
National Institute of Diabetes and Digestive and Kidney Diseases
Eating & Nutrition for Hemodialysis | Preparation
-
Mayo Clinic
Hemodialysis | The Process
-
National Library of Medicine
Hemodialysis | Uses
-
Cleveland Clinic
Dialysis | Disadvantages
-
International Society of Nephrology
Pathogenesis and treatment of dialysis hypotension | Complications
-
National Library of Medicine
Anemia of Chronic Renal Disease | Complications
-
National Library of Medicine
Dialysis-related amyloidosis: challenges and solutions | Complications